
151+ Public Health Research Topics [Updated 2024]

The important area of public health research is essential to forming laws, influencing medical procedures, and eventually enhancing community well-being. As we delve into the vast landscape of public health research topics, it’s essential to understand the profound impact they have on society.
This blog aims to provide a comprehensive guide to selecting and understanding the diverse array of public health research topics.
Overview of Public Health Research Topics
Table of Contents
Public health research encompasses a wide range of subjects, reflecting the interdisciplinary nature of the field. From epidemiology and health policy to environmental health and infectious diseases, researchers navigate through various dimensions to address complex health challenges.
Each category holds its own significance, contributing to the overall understanding of public health dynamics.
Key Considerations in Selecting Public Health Research Topics
- Current Relevance: Assess the timeliness of potential topics by considering recent health trends, emerging issues, and societal concerns.
- Impact on Public Health: Evaluate the potential impact of the research on improving health outcomes, addressing disparities, or influencing policy and interventions.
- Feasibility and Resources: Gauge the practicality of conducting research on a particular topic, considering available resources, data accessibility, and research infrastructure.
- Ethical Considerations: Scrutinize the ethical implications of the research, ensuring it aligns with ethical standards and guidelines, especially when dealing with vulnerable populations or sensitive topics.
Top 151+ Public Health Research Topics
Epidemiology.
- The Impact of Social Determinants on Disease Outcomes
- Patterns and Trends in Emerging Infectious Diseases
- Investigating Health Disparities among Different Ethnic Groups
- Childhood Obesity and its Long-Term Health Consequences
- Assessing the Effectiveness of Contact Tracing in Disease Control
Health Policy
- Universal Healthcare: Comparative Analysis of Global Models
- The Role of Telemedicine in Improving Healthcare Access
- Evaluating Mental Health Policies and Their Impact on Communities
- Assessing the Impact of Affordable Care Act on Public Health
- Vaccine Policies and Public Perception: A Comprehensive Study
Environmental Health
- Climate Change and Health: Adapting to the Challenges
- Air Quality and Respiratory Health in Urban Environments
- Waterborne Diseases and Strategies for Safe Water Supply
- Occupational Health Hazards: A Comprehensive Workplace Analysis
- The Impact of Green Spaces on Mental Health in Urban Areas
Infectious Diseases
- Antimicrobial Resistance: Strategies for Mitigation
- Vaccination Strategies and Herd Immunity
- Global Health Security: Preparedness for Pandemics
- The Impact of Vector-Borne Diseases on Public Health
- Emerging Trends in Antibiotic-Resistant Infections
Chronic Diseases
- Lifestyle Interventions for Preventing Cardiovascular Diseases
- Genetic Factors in the Development of Cancer: A Comprehensive Study
- Aging and Health: Addressing the Healthcare Needs of the Elderly
- Diabetes Prevention Programs: Efficacy and Implementation
- Mental Health in Chronic Disease Patients: Bridging the Gap
Maternal and Child Health
- Maternal Mortality: Understanding Causes and Prevention
- The Impact of Breastfeeding on Infant Health and Development
- Childhood Immunization: Barriers and Strategies for Improvement
- Teenage Pregnancy and Its Long-Term Health Consequences
- Mental Health Support for Postpartum Women: Current Gaps and Solutions
Health Behavior and Promotion
- Smoking Cessation Programs: Effectiveness and Challenges
- Physical Activity Promotion in Schools: Strategies for Success
- Nutrition Education and Its Impact on Healthy Eating Habits
- Mental Health Awareness Campaigns: Assessing Public Perceptions
- The Role of Social Media in Health Promotion
Global Health
- Assessing the Impact of International Aid on Global Health
- Water, Sanitation, and Hygiene (WASH) Programs in Developing Countries
- The Role of Non-Governmental Organizations in Global Health
- Communicable Disease Control in Refugee Populations
- Global Access to Essential Medicines: Challenges and Solutions
Community Health
- Community-Based Participatory Research: Best Practices and Challenges
- The Impact of Community Health Workers on Health Outcomes
- Health Literacy and its Relationship to Health Disparities
- Assessing the Effectiveness of Mobile Health (mHealth) Interventions
- Community Resilience in the Face of Public Health Crises
Healthcare Quality and Patient Safety
- Hospital-Acquired Infections: Strategies for Prevention
- Patient Safety Culture in Healthcare Organizations
- Quality Improvement Initiatives in Primary Care Settings
- Healthcare Accreditation: Impact on Patient Outcomes
- Implementing Electronic Health Records: Challenges and Benefits
Mental Health
- Stigma Reduction Programs for Mental Health Disorders
- Integrating Mental Health into Primary Care Settings
- The Impact of COVID-19 on Mental Health: Long-Term Implications
- Mental Health in the Workplace: Strategies for Employee Well-being
- Suicide Prevention Programs: Effectiveness and Outreach
Health Disparities
- Racial Disparities in Healthcare: Addressing Systemic Inequities
- LGBTQ+ Health Disparities and Inclusive Healthcare Practices
- Socioeconomic Status and Access to Healthcare Services
- Geographical Disparities in Health: Rural vs. Urban
- The Impact of Gender on Health Outcomes and Access to Care
Public Health Education
- Evaluation of Public Health Education Programs
- Innovative Approaches to Teaching Public Health Concepts
- Online Health Education Platforms: Opportunities and Challenges
- Interdisciplinary Training in Public Health: Bridging Gaps
- Continuing Education for Public Health Professionals: Current Landscape
Digital Health
- The Role of Wearable Devices in Health Monitoring
- Telehealth Adoption: Barriers and Opportunities
- Health Apps for Chronic Disease Management: User Perspectives
- Blockchain Technology in Healthcare: Privacy and Security Implications
- Artificial Intelligence in Disease Diagnosis and Prediction
Health Economics
- Cost-Effectiveness of Preventive Health Interventions
- The Impact of Healthcare Financing Models on Access to Care
- Pharmaceutical Pricing and Access to Essential Medicines
- Economic Evaluation of Health Promotion Programs
- Health Insurance Coverage and Health Outcomes: A Global Perspective
Innovations in Public Health
- 3D Printing in Healthcare: Applications and Future Prospects
- Gene Editing Technologies and their Ethical Implications
- Smart Cities and Public Health: Integrating Technology for Well-being
- Nanotechnology in Medicine: Potential for Disease Treatment
- The Role of Drones in Public Health: Surveillance and Intervention
Food Safety and Nutrition
- Foodborne Illness Outbreaks: Investigating Causes and Prevention
- Sustainable Food Systems: Implications for Public Health
- Nutritional Interventions for Malnutrition in Developing Countries
- Food Labeling and Consumer Understanding: A Critical Review
- The Impact of Fast Food Consumption on Public Health
Substance Abuse
- Opioid Epidemic: Strategies for Prevention and Treatment
- Harm Reduction Approaches in Substance Abuse Programs
- Alcohol Consumption Patterns and Public Health Outcomes
- Smoking and Mental Health: Exploring the Connection
- Novel Psychoactive Substances: Emerging Threats and Strategies
Occupational Health
- Workplace Stress and Mental Health: Intervention Strategies
- Occupational Hazards in Healthcare Professions: A Comparative Analysis
- Ergonomics in the Workplace: Improving Worker Health and Productivity
- Night Shift Work and Health Consequences: Addressing Challenges
- Occupational Health and Safety Regulations: A Global Overview
Disaster Preparedness and Response
- Pandemic Preparedness and Lessons from COVID-19
- Natural Disasters and Mental Health: Post-Traumatic Stress
- Emergency Response Systems: Improving Timeliness and Efficiency
- Communicating Health Risks During Emergencies: Public Perception
- Collaborative Approaches to Disaster Response in Global Health
Cancer Research
- Precision Medicine in Cancer Treatment: Current Advancements
- Cancer Screening Programs: Efficacy and Challenges
- Environmental Factors and Cancer Risk: Exploring Connections
- Survivorship Care Plans: Enhancing Quality of Life after Cancer
- Integrative Therapies in Cancer Care: Complementary Approaches
Sexual and Reproductive Health
- Access to Contraception in Developing Countries: Challenges and Solutions
- Comprehensive Sex Education Programs: Impact on Teen Pregnancy
- Reproductive Health Rights: Global Perspectives and Challenges
- Infertility Treatment: Ethical Considerations and Societal Impact
- Maternal and Child Health in Conflict Zones: Addressing Challenges
Cardiovascular Health
- Hypertension Prevention Programs: Strategies and Effectiveness
- Cardiovascular Disease in Women: Gender-Specific Risk Factors
- Innovations in Cardiac Rehabilitation Programs
- Artificial Heart Technology: Advancements and Ethical Implications
- Impact of Air Pollution on Cardiovascular Health: A Global Concern
Social Determinants of Health
- Educational Attainment and Health Outcomes: Exploring Links
- Income Inequality and its Impact on Population Health
- Social Support Networks and Mental Health: A Comprehensive Study
- Neighborhood Environments and Health Disparities
- Employment and Health: The Interplay of Work and Well-being
Genomics and Public Health
- Population Genomics and its Implications for Public Health
- Genetic Counseling and Education: Empowering Individuals and Families
- Ethical Issues in Genetic Research: Privacy and Informed Consent
- Pharmacogenomics: Tailoring Drug Therapies to Individual Genotypes
- Gene-Environment Interactions in Disease Risk: Unraveling Complexities
Public Health Ethics
- Informed Consent in Public Health Research: Current Practices
- Ethical Challenges in Global Health Research: Balancing Priorities
- Confidentiality in Public Health Reporting: Striking the Right Balance
- Research with Vulnerable Populations: Ethical Considerations
- Ethical Implications of Emerging Technologies in Healthcare
Health Communication
- The Role of Media in Shaping Public Health Perceptions
- Health Literacy Interventions: Improving Understanding of Health Information
- Social Media Campaigns for Public Health Promotion: Best Practices
- Tailoring Health Messages for Diverse Audiences: Cultural Competency
- Risk Communication in Public Health Emergencies: Lessons Learned
Nutrigenomics
- Personalized Nutrition Plans based on Genetic Makeup
- Impact of Nutrigenomics on Chronic Disease Prevention
- Ethical Considerations in Nutrigenomics Research
- Public Perceptions of Nutrigenomic Testing: A Qualitative Study
- Integrating Nutrigenomics into Public Health Policies
Public Health and Artificial Intelligence
- Predictive Analytics in Disease Surveillance: Harnessing AI for Early Detection
- Ethical Considerations in AI-Driven Health Decision Support Systems
- Machine Learning in Epidemiology: Predicting Disease Outbreaks
- Natural Language Processing in Public Health: Text Mining for Insights
- Bias in AI Algorithms: Implications for Health Equity
Health Disparities in Aging
- Geriatric Health Disparities: Bridging the Gap in Elderly Care
- Ageism in Healthcare: Addressing Stereotypes and Discrimination
- Social Isolation and Health Consequences in Aging Populations
- Access to Palliative Care for Older Adults: A Global Perspective
- Alzheimer’s Disease and Ethnic Disparities in Diagnosis and Treatment
- Loneliness and Mental Health in the Elderly: Interventions and Support
Research Methodologies in Public Health
Public health research employs various methodologies, including quantitative, qualitative, and mixed-methods approaches. Each method brings its own strengths to the research process, allowing researchers to gain a comprehensive understanding of the complex issues they investigate.
Community-based participatory research is another valuable approach, emphasizing collaboration with communities to address their specific health concerns.
Challenges and Opportunities in Public Health Research
While public health research is immensely rewarding, it comes with its own set of challenges. Funding constraints, ethical dilemmas, the need for interdisciplinary collaboration, and the integration of technology pose both obstacles and opportunities.
Researchers must navigate these challenges to ensure their work has a meaningful impact on public health.
In conclusion, public health research topics are diverse and dynamic, reflecting the complex nature of the field. As researchers embark on their journeys, they must carefully consider the relevance, impact, and ethical implications of their chosen topics.
The collaborative and interdisciplinary nature of public health research positions it as a powerful tool in addressing the health challenges of our time. By exploring the depths of these topics, researchers contribute to the collective effort to build healthier and more equitable communities.
As we move forward, a continued exploration of relevant public health research topics is essential for shaping the future of healthcare and improving the well-being of populations worldwide.
Related Posts

Step by Step Guide on The Best Way to Finance Car

The Best Way on How to Get Fund For Business to Grow it Efficiently
- Search Menu
- Sign in through your institution
- Browse content in Arts and Humanities
- Browse content in Archaeology
- Prehistoric Archaeology
- Browse content in Art
- History of Art
- Browse content in Classical Studies
- Classical History
- Classical Literature
- Classical Reception
- Greek and Roman Archaeology
- Digital Humanities
- Browse content in History
- Diplomatic History
- Environmental History
- Genocide and Ethnic Cleansing
- History by Period
- Legal and Constitutional History
- Regional and National History
- Social and Cultural History
- Theory, Methods, and Historiography
- World History
- Browse content in Language Teaching and Learning
- Language Teaching Theory and Methods
- Browse content in Linguistics
- Applied Linguistics
- Language Evolution
- Language Families
- Lexicography
- Browse content in Literature
- Bibliography
- Literary Studies (American)
- Literary Studies (20th Century onwards)
- Literary Studies (British and Irish)
- Literary Studies (Women's Writing)
- Literary Theory and Cultural Studies
- Shakespeare Studies and Criticism
- Browse content in Media Studies
- Browse content in Music
- Applied Music
- Medicine and Music
- Music Theory and Analysis
- Musical Structures, Styles, and Techniques
- Musicology and Music History
- Browse content in Philosophy
- Aesthetics and Philosophy of Art
- Epistemology
- History of Western Philosophy
- Metaphysics
- Moral Philosophy
- Philosophy of Mind
- Philosophy of Science
- Philosophy of Mathematics and Logic
- Practical Ethics
- Browse content in Religion
- Christianity
- Judaism and Jewish Studies
- Religion and Science
- Religion and Law
- Religion and Art, Literature, and Music
- Religious Studies
- Browse content in Society and Culture
- Ethical Issues and Debates
- Browse content in Law
- Arbitration
- Company and Commercial Law
- Comparative Law
- Competition Law
- Browse content in Constitutional and Administrative Law
- Parliamentary and Legislative Practice
- Employment and Labour Law
- Environment and Energy Law
- Financial Law
- History of Law
- Human Rights and Immigration
- Intellectual Property Law
- Browse content in International Law
- Private International Law and Conflict of Laws
- Public International Law
- IT and Communications Law
- Jurisprudence and Philosophy of Law
- Law and Society
- Legal System and Practice
- Medical and Healthcare Law
- Browse content in Medicine and Health
- Browse content in Allied Health Professions
- Dietetics and Nutrition
- Physiotherapy
- Radiography
- Anaesthetics
- Clinical Neuroscience
- Browse content in Clinical Medicine
- Acute Medicine
- Cardiovascular Medicine
- Clinical Pharmacology and Therapeutics
- Dermatology
- Endocrinology and Diabetes
- Gastroenterology
- Geriatric Medicine
- Infectious Diseases
- Medical Toxicology
- Medical Oncology
- Rheumatology
- Sleep Medicine
- Community Medical Services
- Critical Care
- Forensic Medicine
- History of Medicine
- Medical Skills
- Browse content in Medical Dentistry
- Restorative Dentistry and Orthodontics
- Medical Ethics
- Medical Statistics and Methodology
- Browse content in Neurology
- Neuropathology
- Nursing Studies
- Browse content in Obstetrics and Gynaecology
- Gynaecology
Occupational Medicine
- Paediatrics
- Browse content in Pathology
- Clinical Cytogenetics and Molecular Genetics
- Medical Microbiology and Virology
- Patient Education and Information
- Browse content in Pharmacology
- Psychopharmacology
- Browse content in Preclinical Medicine
- Molecular Biology and Genetics
- Reproduction, Growth and Development
- Primary Care
- Professional Development in Medicine
- Browse content in Psychiatry
- Child and Adolescent Psychiatry
- Forensic Psychiatry
- Browse content in Public Health and Epidemiology
- Epidemiology
- Public Health
- Browse content in Radiology
- Clinical Radiology
- Interventional Radiology
- Radiation Oncology
- Reproductive Medicine
- Browse content in Surgery
- Cardiothoracic Surgery
- Gastro-intestinal and Colorectal Surgery
- Neurosurgery
- Plastic and Reconstructive Surgery
- Trauma and Orthopaedic Surgery
- Browse content in Science and Mathematics
- Browse content in Biological Sciences
- Aquatic Biology
- Biochemistry
- Bioinformatics and Computational Biology
- Developmental Biology
- Ecology and Conservation
- Evolutionary Biology
- Genetics and Genomics
- Microbiology
- Molecular and Cell Biology
- Plant Sciences and Forestry
- Research Methods in Life Sciences
- Structural Biology
- Systems Biology
- Zoology and Animal Sciences
- Browse content in Chemistry
- Medicinal Chemistry
- Mineralogy and Gems
- Physical Chemistry
- Browse content in Computer Science
- Artificial Intelligence
- Computer Architecture and Logic Design
- Human-Computer Interaction
- Mathematical Theory of Computation
- Browse content in Computing
- Computer Security
- Computer Networking and Communications
- Browse content in Earth Sciences and Geography
- Atmospheric Sciences
- Environmental Geography
- Geology and the Lithosphere
- Meteorology and Climatology
- Browse content in Engineering and Technology
- Agriculture and Farming
- Biological Engineering
- Civil Engineering, Surveying, and Building
- Energy Technology
- Engineering (General)
- Environmental Science, Engineering, and Technology
- Transport Technology and Trades
- Browse content in Environmental Science
- Environmental Sustainability
- Management of Land and Natural Resources (Environmental Science)
- Browse content in Materials Science
- Ceramics and Glasses
- Composite Materials
- Nanotechnology
- Browse content in Mathematics
- Applied Mathematics
- Biomathematics and Statistics
- Mathematical Education
- Mathematical Analysis
- Probability and Statistics
- Pure Mathematics
- Browse content in Neuroscience
- Cognition and Behavioural Neuroscience
- Neuroscientific Techniques
- Browse content in Physics
- Astronomy and Astrophysics
- Classical Mechanics
- Relativity and Gravitation
- Browse content in Psychology
- Clinical Psychology
- Cognitive Psychology
- Cognitive Neuroscience
- Health Psychology
- Music Psychology
- Neuropsychology
- Organizational Psychology
- Browse content in Social Sciences
- Browse content in Anthropology
- Human Evolution
- Browse content in Business and Management
- Human Resource Management
- Industrial and Employment Relations
- Industry Studies
- Information and Communication Technologies
- Organizational Theory and Behaviour
- Public and Nonprofit Management
- Browse content in Criminology and Criminal Justice
- Criminology
- Browse content in Economics
- Agricultural, Environmental, and Natural Resource Economics
- Behavioural Economics and Neuroeconomics
- Econometrics and Mathematical Economics
- Economic History
- Economic Development and Growth
- Financial Markets
- Financial Institutions and Services
- Health, Education, and Welfare
- Labour and Demographic Economics
- Law and Economics
- Public Economics
- Urban, Rural, and Regional Economics
- Browse content in Education
- Schools Studies
- Teaching of Specific Groups and Special Educational Needs
- Environment
- Browse content in Human Geography
- Economic Geography
- Browse content in Interdisciplinary Studies
- Communication Studies
- Museums, Libraries, and Information Sciences
- Browse content in Politics
- Foreign Policy
- Gender and Politics
- International Relations
- International Organization (Politics)
- Political Behaviour
- Political Economy
- Political Institutions
- Political Sociology
- Political Theory
- Public Policy
- Public Administration
- Quantitative Political Methodology
- Regional Political Studies
- Security Studies
- Browse content in Regional and Area Studies
- African Studies
- Japanese Studies
- Research and Information
- Browse content in Social Work
- Addictions and Substance Misuse
- Browse content in Sociology
- Economic Sociology
- Gender and Sexuality
- Gerontology and Ageing
- Health, Illness, and Medicine
- Migration Studies
- Race and Ethnicity
- Social Movements and Social Change
- Social Research and Statistics
- Social Stratification, Inequality, and Mobility
- Sociology of Religion
- Urban and Rural Studies
- Journals A to Z
- Books on Oxford Academic
What are the trending topics in Public Health and related disciplines?
You can identify some of the most discussed and influential topics with the help of Altmetric attention scores, which take into account several outlets including social media, news articles, and policy documents.
Drawing from a selection of Public Health and Medicine journals, we have compiled a list of the articles that have been mentioned the most over the past few months.
Discover the articles that are trending right now, and catch up on current topics in Public Health and related disciplines. We will update our collection every few weeks; come back to this page to be on top of the latest conversations in Public Health and Medicine. Previously featured articles are listed here .
You can also sign up for e-alerts to make sure you never miss the latest research from our journals.
*Last updated October 2021*
Age and Ageing
Alcohol and alcoholism, american journal of epidemiology, annals of work exposures and health, epidemiologic reviews, european journal of public health, family practice, health education research, health policy and planning, health promotion international, international health, international journal of epidemiology, international journal for quality in health care, journal of public health, journal of travel medicine, journal of tropical pediatrics, nicotine & tobacco research, transactions of the royal society of tropical medicine & hygiene, behaviour change interventions to increase physical activity in hospitalised patients: a systematic review, meta-analysis and meta-regression.
There is moderate-certainty evidence that behaviour change interventions are associated with increased physical activity levels among older hospitalised patients.
Attention-Deficit/Hyperactivity Disorder and Alcohol and Other Substance Use Disorders in Young Adulthood: Findings from a Canadian Nationally Representative Survey
This study from Canada found that one in three young adults with ADHD had a lifetime alcohol use disorder, and that young adults with ADHD were also three times more likely to develop a substance use disorder. Targeted outreach and interventions for this extremely vulnerable population are warranted.
Expiring Eviction Moratoriums and COVID-19 Incidence and Mortality
According to this study, resuming evictions in summer 2020 was associated with increased COVID-19 incidence and mortality in US states, with an estimated 433,700 excess cases and 10,700 excess deaths. Explore more research on COVID-19 in a curated collection from the AJE: https://academic.oup.com/aje/pages/covid-19
The Development of a Covid-19 Control Measures Risk Matrix for Occupational Hygiene Protective Measures
The British Occupational Hygiene Society (BOHS) developed a control banding matrix for employers and others to help assess the risks of COVID-19 infection, and calls for further work to validate the reliability of the tool. Browse the Annals' collection on occupational hygiene for virus protection: https://academic.oup.com/annweh/pages/covid-19
Immunization to Protect the US Armed Forces: Heritage, Current Practice, and Prospects
In 1777, George Washington ordered a mandatory inoculation program for his troops, in what would become the first mass immunization mandate in the US. This archival article discussess and contextualizes immunization practices for US Armed Forces.
Does face mask use elicit risk-compensation? Quasi-experimental evidence from Denmark during the SARS-CoV-2 pandemic
Responding to concerns that that face mask use could elicit a false sense of security and lead to riskier behaviours, this study from Denmark found that mask use overall correlated positively with protective behaviours.
Evidence reversals in primary care research: a study of randomized controlled trials
While medical practice is often undermined by subsequent investigation, randomized trials relevant to primary care generally hold up over time.
Social media influencers can be used to deliver positive information about the flu vaccine: findings from a multi-year study
This study shows the potential for using social media influencers to inspire positive engagements on pro-vaccine health messaging. For more content on accurate information's importance for public health, browse the latest article collection from HER: https://academic.oup.com/her/pages/covid-19
COVID-19 Preparedness and Response Plans from 106 countries: a review from a health systems resilience perspective
Current emergency response planning does not have adequate coverage to maintain health systems functionality for essential health service delivery alongside emergency-specific interventions and healthcare. The findings from this study can help align health emergency planning with broader population health needs.
Rise and demise: a case study of public health nutrition in Queensland, Australia, over three decades
This case study shows that that ongoing efforts are needed to improve sustainability of nutrition policy and programmes to address all diet-related diseases.
Institutional and behaviour-change interventions to support COVID-19 public health measures: a review by the Lancet Commission Task Force on public health measures to suppress the pandemic
This review article outlines evidence for a range of institutional measures and behaviour-change measures, and highlights research and knowledge gaps.
Quantifying impacts of the COVID-19 pandemic through life-expectancy losses: a population-level study of 29 countries
The COVID-19 pandemic triggered significant mortality increases in 2020 of a magnitude not witnessed since World War II in Western Europe or the breakup of the Soviet Union in Eastern Europe.
Gender in the Consolidated Criteria for Reporting Qualitative Research (COREQ) Checklist
The authors propose an update to the Equator’s Consolidated criteria for reporting qualitative research (COREQ) checklist, with the aim of enhancing inclusivity.
Rate of reinfections after SARS-CoV-2 primary infection in the population of an Italian province: a cohort study
This study confirms previous findings on a low risk of SARS-CoV-2 reinfection. If confirmed, these findings suggest that more targeted restriction policies can be applied to the subjects that recovered after a first infection. Read highly cited papers on COVID-19 from the Journal of Public Health: https://academic.oup.com/jpubhealth/pages/covid-19
The reproductive number of the Delta variant of SARS-CoV-2 is far higher compared to the ancestral SARS-CoV-2 virus
Given the Delta variant's high reproductive number associated with higher transmissibility, in a context of globally still low vaccine coverage rates and lower vaccine effectiveness, public health and social measures will need to be substantially strengthened. A high reproductive number also means that much higher vaccine coverage rates need to be achieved compared to the originally assumed.
Neurological Complications of SARS-CoV-2 Infection in Children: A Systematic Review and Meta-Analysis
Neurological complications are rare in children suffering from COVID-19. Still, these children are at risk of developing seizures and encephalopathy, more in those suffering from severe illness.
Reactions to Sales Restrictions on Flavored Vape Products or All Vape Products Among Young Adults in the United States
The researchers examined support for and perceived impact of e-cigarette sales restrictions. Findings suggest that bans on flavored vape products could have a positive impact on lower-risk users, but that other young adult user subgroups may not experience benefit.
Covid-19 and Health at Work
An editorial from the earlier stages of the pandemic highlights the importance of properly fitted respirators for worker safety and outlines occupational hygiene measures.
Lessons from the field: delivering trachoma mass drug administration safely in a COVID-19 context
Guidelines for safe mass drug administration for neglected tropical diseases were developed in a COVID-19 context; training and implementation were assessed through an observation checklist.
For more research on the impact of COVID-19 on NTDs, explore the March 2021 special issue: https://academic.oup.com/trstmh/issue/115/3
Previously featured
Age and frailty are independently associated with increased COVID-19 mortality and increased care needs in survivors: results of an international multi-centre study
Trajectories of Alcohol Use and Related Harms for Managed Alcohol Program Participants over 12 Months Compared with Local Controls: A Quasi-Experimental Study
Estimating the Effect of Social Distancing Interventions on COVID-19 in the United States
Selecting Controls for Minimizing SARS-CoV-2 Aerosol Transmission in Workplaces and Conserving Respiratory Protective Equipment Supplies
What Do We Know About the Association Between Firearm Legislation and Firearm-Related Injuries?
Denialism: what is it and how should scientists respond?
Acute cooling of the feet and the onset of common cold symptoms
The effect of falsely balanced reporting of the autism–vaccine controversy on vaccine safety perceptions and behavioral intentions
Climate change: an urgent priority for health policy and systems research
Power, control, communities and health inequalities I: theories, concepts and analytical frameworks
Research ethics in context: understanding the vulnerabilities, agency and resourcefulness of research participants living along the Thai–Myanmar border
Tobacco smoking and mortality among Aboriginal and Torres Strait Islander adults in Australia
Quality and safety in the time of Coronavirus: design better, learn faster
Years of life lost associated with COVID-19 deaths in the United States
In-flight transmission of SARS-CoV-2: a review of the attack rates and available data on the efficacy of face masks
Stability of the Initial Diagnosis of Autism Spectrum Disorder by DSM-5 in Children: A Short-Term Follow-Up Study
Impact of Tobacco Smoking on the Risk of COVID-19: A Large Scale Retrospective Cohort Study
Mental health of staff working in intensive care during COVID-19
The benefits and costs of social distancing in high- and low-income countries
A classification tree to assist with routine scoring of the Clinical Frailty Scale
Recent Advances in the Potential of Positive Allosteric Modulators of the GABAB Receptor to Treat Alcohol Use Disorder
The recent oubreak of smallpox in Meschede, West Germany
Your Hair or Your Service: An Issue of Faith for Sikh Healthcare Professionals During the COVID-19 Pandemic
Emerging Infections: Pandemic Influenza
Identifying the views of adolescents in five European countries on the drivers of obesity using group model building
Novel multi-virus rapid respiratory microbiological point-of-care testing in primary care: a mixed-methods feasibility evaluation
Public health crisis in the refugee community: little change in social determinants of health preserve health disparities
In search of ‘community’: a critical review of community mental health services for women in African settings
COVID-19, a tale of two pandemics: novel coronavirus and fake news messaging
Disrupting vaccine logistics
Use of directed acyclic graphs (DAGs) to identify confounders in applied health research: review and recommendations
Measurement and monitoring patient safety in prehospital care: a systematic review
Black Lives Matter protests and COVID-19 cases: relationship in two databases
The positive impact of lockdown in Wuhan on containing the COVID-19 outbreak in China
Severe Malnutrition and Anemia Are Associated with Severe COVID in Infants
A Single-Arm, Open-Label, Pilot, and Feasibility Study of a High Nicotine Strength E-Cigarette Intervention for Smoking Cessation or Reduction for People With Schizophrenia Spectrum Disorders Who Smoke Cigarettes
Healthcare workers and protection against inhalable SARS-CoV-2 aerosols
Affiliations
- Copyright © 2024
- About Oxford Academic
- Publish journals with us
- University press partners
- What we publish
- New features
- Open access
- Institutional account management
- Rights and permissions
- Get help with access
- Accessibility
- Advertising
- Media enquiries
- Oxford University Press
- Oxford Languages
- University of Oxford
Oxford University Press is a department of the University of Oxford. It furthers the University's objective of excellence in research, scholarship, and education by publishing worldwide
- Copyright © 2024 Oxford University Press
- Cookie settings
- Cookie policy
- Privacy policy
- Legal notice
This Feature Is Available To Subscribers Only
Sign In or Create an Account
This PDF is available to Subscribers Only
For full access to this pdf, sign in to an existing account, or purchase an annual subscription.
An official website of the United States government
Here’s how you know
Official websites use .gov A .gov website belongs to an official government organization in the United States.
Secure .gov websites use HTTPS A lock ( A locked padlock ) or https:// means you’ve safely connected to the .gov website. Share sensitive information only on official, secure websites.
Global Health Research Topics
Subscribe to Fogarty's Global Health Matters newsletter , and weekly funding news for global health researchers .

The Fogarty International Center and its NIH partners invest in research on a variety of topics vital to global health. For each of these global health research topics, find an in-depth collection of news, resources and funding from Fogarty, the NIH, other U.S. government agencies, nongovernmental organizations and others.
- Chronic noncommunicable diseases (NCDs)
- Climate change
- Deafness and other communication disorders
- Diversity, equity, inclusion, and accessibility
- Eye disease, vision health and blindness
- Global health security
- Household air pollution
- Implementation science
- Infectious diseases
- Coronaviruses
- Ebola virus disease
- Tuberculosis (TB)
- Maternal and child health
- Mentoring and mentorship training
- Mobile health (mHealth)
- Neurological and mental disorders and diseases
- Oral and dental health
- Trauma and injury
- Tobacco control
- Women’s leadership in global health research
Health Topic Information
- NIH Health Topics
- MedlinePlus Health Topics
- Diseases and Conditions from the U.S. Centers for Disease Control and Prevention (CDC)
Updated January 3, 2024
Thank you for visiting nature.com. You are using a browser version with limited support for CSS. To obtain the best experience, we recommend you use a more up to date browser (or turn off compatibility mode in Internet Explorer). In the meantime, to ensure continued support, we are displaying the site without styles and JavaScript.
- View all journals
Public health articles from across Nature Portfolio
Public health is the medical discipline concerned with the prevention and control of disease through population surveillance and the promotion of healthy behaviours. Strategies used to promote public health include patient education, the administration of vaccines, and other components of preventive medicine.

Food fortification programmes and zinc deficiency
The complex realities of most countries grappling with zinc deficiency pose challenges to the implementation of highly compliant, mandatory, large-scale food fortification programmes.
- Nicola M. Lowe
- Swarnim Gupta
Related Subjects
- Epidemiology
- Population screening
Latest Research and Reviews
Follow-up of telemedicine mental health interventions amid COVID-19 pandemic
- Carlos Roncero
- Sara Díaz-Trejo
- Armando González-Sánchez
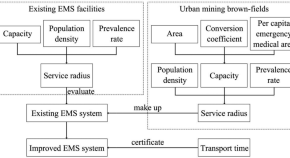
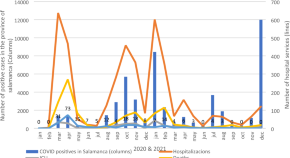
Improving urban emergency medical service systems through brownfield transformation in Huangshi, China
- Zhiping Liu
- Yingxue Feng
The VRF-L and VRF-GL IOL power calculation methods after radial keratotomy
- Oleksiy V. Voytsekhivskyy
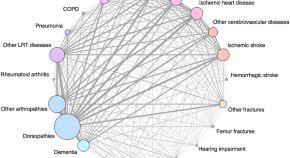
Clinical subtypes of older adults starting long-term care in Japan and their association with prognoses: a data-driven cluster analysis
- Masao Iwagami
- Nanako Tamiya
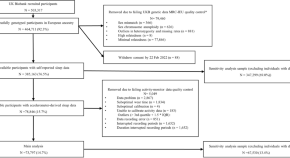
The role of accelerometer-derived sleep traits on glycated haemoglobin and glucose levels: a Mendelian randomization study
- Rebecca C. Richmond
- Deborah A. Lawlor
Contextual and individual inequalities in breast cancer screening participation and outcomes in Turin (North-West Italy)
- Chiara Di Girolamo
- Giulio Cammarata
- Fulvio Ricceri
News and Comment

Combined COVID-flu vaccines are coming: Moderna jab clears major test
First large trial suggests mRNA drug gives better protection from SARS-CoV-2 and influenza viruses than single-target shots.
- Freda Kreier

‘Vindicated’: Embattled misinformation researchers celebrate key US Supreme Court decision
The justices rule that the US government can keep talking to scientists and social-media firms with the aim of curbing falsehoods online.
- Jeff Tollefson
Establish a global day to tackle postpartum haemorrhage
- Abdulhammed Opeyemi Babatunde
- Abdullahi Tunde Aborode
- Oladapo O. Olayemi

How climate change is hitting Europe: three graphics reveal health impacts
A growing body of research reveals the deaths and diseases linked to rising temperatures across the continent.
- Carissa Wong
Decolonizing global health by engineering equitable relationships
Global health-related research and development continues to uphold colonialist structures, concentrating knowledge generation and innovation to high-income countries, thereby hindering global health equity. Therefore, in addition to engineering new technologies, bioengineers will need to try to engineer equitable relationships.
Quick links
- Explore articles by subject
- Guide to authors
- Editorial policies
Research Topics & Ideas: Healthcare
100+ Healthcare Research Topic Ideas To Fast-Track Your Project

Finding and choosing a strong research topic is the critical first step when it comes to crafting a high-quality dissertation, thesis or research project. If you’ve landed on this post, chances are you’re looking for a healthcare-related research topic , but aren’t sure where to start. Here, we’ll explore a variety of healthcare-related research ideas and topic thought-starters across a range of healthcare fields, including allopathic and alternative medicine, dentistry, physical therapy, optometry, pharmacology and public health.
NB – This is just the start…
The topic ideation and evaluation process has multiple steps . In this post, we’ll kickstart the process by sharing some research topic ideas within the healthcare domain. This is the starting point, but to develop a well-defined research topic, you’ll need to identify a clear and convincing research gap , along with a well-justified plan of action to fill that gap.
If you’re new to the oftentimes perplexing world of research, or if this is your first time undertaking a formal academic research project, be sure to check out our free dissertation mini-course. In it, we cover the process of writing a dissertation or thesis from start to end. Be sure to also sign up for our free webinar that explores how to find a high-quality research topic.
Overview: Healthcare Research Topics
- Allopathic medicine
- Alternative /complementary medicine
- Veterinary medicine
- Physical therapy/ rehab
- Optometry and ophthalmology
- Pharmacy and pharmacology
- Public health
- Examples of healthcare-related dissertations
Allopathic (Conventional) Medicine
- The effectiveness of telemedicine in remote elderly patient care
- The impact of stress on the immune system of cancer patients
- The effects of a plant-based diet on chronic diseases such as diabetes
- The use of AI in early cancer diagnosis and treatment
- The role of the gut microbiome in mental health conditions such as depression and anxiety
- The efficacy of mindfulness meditation in reducing chronic pain: A systematic review
- The benefits and drawbacks of electronic health records in a developing country
- The effects of environmental pollution on breast milk quality
- The use of personalized medicine in treating genetic disorders
- The impact of social determinants of health on chronic diseases in Asia
- The role of high-intensity interval training in improving cardiovascular health
- The efficacy of using probiotics for gut health in pregnant women
- The impact of poor sleep on the treatment of chronic illnesses
- The role of inflammation in the development of chronic diseases such as lupus
- The effectiveness of physiotherapy in pain control post-surgery

Topics & Ideas: Alternative Medicine
- The benefits of herbal medicine in treating young asthma patients
- The use of acupuncture in treating infertility in women over 40 years of age
- The effectiveness of homoeopathy in treating mental health disorders: A systematic review
- The role of aromatherapy in reducing stress and anxiety post-surgery
- The impact of mindfulness meditation on reducing high blood pressure
- The use of chiropractic therapy in treating back pain of pregnant women
- The efficacy of traditional Chinese medicine such as Shun-Qi-Tong-Xie (SQTX) in treating digestive disorders in China
- The impact of yoga on physical and mental health in adolescents
- The benefits of hydrotherapy in treating musculoskeletal disorders such as tendinitis
- The role of Reiki in promoting healing and relaxation post birth
- The effectiveness of naturopathy in treating skin conditions such as eczema
- The use of deep tissue massage therapy in reducing chronic pain in amputees
- The impact of tai chi on the treatment of anxiety and depression
- The benefits of reflexology in treating stress, anxiety and chronic fatigue
- The role of acupuncture in the prophylactic management of headaches and migraines
Topics & Ideas: Dentistry
- The impact of sugar consumption on the oral health of infants
- The use of digital dentistry in improving patient care: A systematic review
- The efficacy of orthodontic treatments in correcting bite problems in adults
- The role of dental hygiene in preventing gum disease in patients with dental bridges
- The impact of smoking on oral health and tobacco cessation support from UK dentists
- The benefits of dental implants in restoring missing teeth in adolescents
- The use of lasers in dental procedures such as root canals
- The efficacy of root canal treatment using high-frequency electric pulses in saving infected teeth
- The role of fluoride in promoting remineralization and slowing down demineralization
- The impact of stress-induced reflux on oral health
- The benefits of dental crowns in restoring damaged teeth in elderly patients
- The use of sedation dentistry in managing dental anxiety in children
- The efficacy of teeth whitening treatments in improving dental aesthetics in patients with braces
- The role of orthodontic appliances in improving well-being
- The impact of periodontal disease on overall health and chronic illnesses

Tops & Ideas: Veterinary Medicine
- The impact of nutrition on broiler chicken production
- The role of vaccines in disease prevention in horses
- The importance of parasite control in animal health in piggeries
- The impact of animal behaviour on welfare in the dairy industry
- The effects of environmental pollution on the health of cattle
- The role of veterinary technology such as MRI in animal care
- The importance of pain management in post-surgery health outcomes
- The impact of genetics on animal health and disease in layer chickens
- The effectiveness of alternative therapies in veterinary medicine: A systematic review
- The role of veterinary medicine in public health: A case study of the COVID-19 pandemic
- The impact of climate change on animal health and infectious diseases in animals
- The importance of animal welfare in veterinary medicine and sustainable agriculture
- The effects of the human-animal bond on canine health
- The role of veterinary medicine in conservation efforts: A case study of Rhinoceros poaching in Africa
- The impact of veterinary research of new vaccines on animal health
Topics & Ideas: Physical Therapy/Rehab
- The efficacy of aquatic therapy in improving joint mobility and strength in polio patients
- The impact of telerehabilitation on patient outcomes in Germany
- The effect of kinesiotaping on reducing knee pain and improving function in individuals with chronic pain
- A comparison of manual therapy and yoga exercise therapy in the management of low back pain
- The use of wearable technology in physical rehabilitation and the impact on patient adherence to a rehabilitation plan
- The impact of mindfulness-based interventions in physical therapy in adolescents
- The effects of resistance training on individuals with Parkinson’s disease
- The role of hydrotherapy in the management of fibromyalgia
- The impact of cognitive-behavioural therapy in physical rehabilitation for individuals with chronic pain
- The use of virtual reality in physical rehabilitation of sports injuries
- The effects of electrical stimulation on muscle function and strength in athletes
- The role of physical therapy in the management of stroke recovery: A systematic review
- The impact of pilates on mental health in individuals with depression
- The use of thermal modalities in physical therapy and its effectiveness in reducing pain and inflammation
- The effect of strength training on balance and gait in elderly patients
Topics & Ideas: Optometry & Opthalmology
- The impact of screen time on the vision and ocular health of children under the age of 5
- The effects of blue light exposure from digital devices on ocular health
- The role of dietary interventions, such as the intake of whole grains, in the management of age-related macular degeneration
- The use of telemedicine in optometry and ophthalmology in the UK
- The impact of myopia control interventions on African American children’s vision
- The use of contact lenses in the management of dry eye syndrome: different treatment options
- The effects of visual rehabilitation in individuals with traumatic brain injury
- The role of low vision rehabilitation in individuals with age-related vision loss: challenges and solutions
- The impact of environmental air pollution on ocular health
- The effectiveness of orthokeratology in myopia control compared to contact lenses
- The role of dietary supplements, such as omega-3 fatty acids, in ocular health
- The effects of ultraviolet radiation exposure from tanning beds on ocular health
- The impact of computer vision syndrome on long-term visual function
- The use of novel diagnostic tools in optometry and ophthalmology in developing countries
- The effects of virtual reality on visual perception and ocular health: an examination of dry eye syndrome and neurologic symptoms
Topics & Ideas: Pharmacy & Pharmacology
- The impact of medication adherence on patient outcomes in cystic fibrosis
- The use of personalized medicine in the management of chronic diseases such as Alzheimer’s disease
- The effects of pharmacogenomics on drug response and toxicity in cancer patients
- The role of pharmacists in the management of chronic pain in primary care
- The impact of drug-drug interactions on patient mental health outcomes
- The use of telepharmacy in healthcare: Present status and future potential
- The effects of herbal and dietary supplements on drug efficacy and toxicity
- The role of pharmacists in the management of type 1 diabetes
- The impact of medication errors on patient outcomes and satisfaction
- The use of technology in medication management in the USA
- The effects of smoking on drug metabolism and pharmacokinetics: A case study of clozapine
- Leveraging the role of pharmacists in preventing and managing opioid use disorder
- The impact of the opioid epidemic on public health in a developing country
- The use of biosimilars in the management of the skin condition psoriasis
- The effects of the Affordable Care Act on medication utilization and patient outcomes in African Americans
Topics & Ideas: Public Health
- The impact of the built environment and urbanisation on physical activity and obesity
- The effects of food insecurity on health outcomes in Zimbabwe
- The role of community-based participatory research in addressing health disparities
- The impact of social determinants of health, such as racism, on population health
- The effects of heat waves on public health
- The role of telehealth in addressing healthcare access and equity in South America
- The impact of gun violence on public health in South Africa
- The effects of chlorofluorocarbons air pollution on respiratory health
- The role of public health interventions in reducing health disparities in the USA
- The impact of the United States Affordable Care Act on access to healthcare and health outcomes
- The effects of water insecurity on health outcomes in the Middle East
- The role of community health workers in addressing healthcare access and equity in low-income countries
- The impact of mass incarceration on public health and behavioural health of a community
- The effects of floods on public health and healthcare systems
- The role of social media in public health communication and behaviour change in adolescents
Examples: Healthcare Dissertation & Theses
While the ideas we’ve presented above are a decent starting point for finding a healthcare-related research topic, they are fairly generic and non-specific. So, it helps to look at actual dissertations and theses to see how this all comes together.
Below, we’ve included a selection of research projects from various healthcare-related degree programs to help refine your thinking. These are actual dissertations and theses, written as part of Master’s and PhD-level programs, so they can provide some useful insight as to what a research topic looks like in practice.
- Improving Follow-Up Care for Homeless Populations in North County San Diego (Sanchez, 2021)
- On the Incentives of Medicare’s Hospital Reimbursement and an Examination of Exchangeability (Elzinga, 2016)
- Managing the healthcare crisis: the career narratives of nurses (Krueger, 2021)
- Methods for preventing central line-associated bloodstream infection in pediatric haematology-oncology patients: A systematic literature review (Balkan, 2020)
- Farms in Healthcare: Enhancing Knowledge, Sharing, and Collaboration (Garramone, 2019)
- When machine learning meets healthcare: towards knowledge incorporation in multimodal healthcare analytics (Yuan, 2020)
- Integrated behavioural healthcare: The future of rural mental health (Fox, 2019)
- Healthcare service use patterns among autistic adults: A systematic review with narrative synthesis (Gilmore, 2021)
- Mindfulness-Based Interventions: Combatting Burnout and Compassionate Fatigue among Mental Health Caregivers (Lundquist, 2022)
- Transgender and gender-diverse people’s perceptions of gender-inclusive healthcare access and associated hope for the future (Wille, 2021)
- Efficient Neural Network Synthesis and Its Application in Smart Healthcare (Hassantabar, 2022)
- The Experience of Female Veterans and Health-Seeking Behaviors (Switzer, 2022)
- Machine learning applications towards risk prediction and cost forecasting in healthcare (Singh, 2022)
- Does Variation in the Nursing Home Inspection Process Explain Disparity in Regulatory Outcomes? (Fox, 2020)
Looking at these titles, you can probably pick up that the research topics here are quite specific and narrowly-focused , compared to the generic ones presented earlier. This is an important thing to keep in mind as you develop your own research topic. That is to say, to create a top-notch research topic, you must be precise and target a specific context with specific variables of interest . In other words, you need to identify a clear, well-justified research gap.
Need more help?
If you’re still feeling a bit unsure about how to find a research topic for your healthcare dissertation or thesis, check out Topic Kickstarter service below.

You Might Also Like:

16 Comments
I need topics that will match the Msc program am running in healthcare research please
Hello Mabel,
I can help you with a good topic, kindly provide your email let’s have a good discussion on this.
Can you provide some research topics and ideas on Immunology?
Thank you to create new knowledge on research problem verse research topic
Help on problem statement on teen pregnancy
This post might be useful: https://gradcoach.com/research-problem-statement/
can you provide me with a research topic on healthcare related topics to a qqi level 5 student
Please can someone help me with research topics in public health ?
Hello I have requirement of Health related latest research issue/topics for my social media speeches. If possible pls share health issues , diagnosis, treatment.
I would like a topic thought around first-line support for Gender-Based Violence for survivors or one related to prevention of Gender-Based Violence
Please can I be helped with a master’s research topic in either chemical pathology or hematology or immunology? thanks
Can u please provide me with a research topic on occupational health and safety at the health sector
Good day kindly help provide me with Ph.D. Public health topics on Reproductive and Maternal Health, interventional studies on Health Education
may you assist me with a good easy healthcare administration study topic
May you assist me in finding a research topic on nutrition,physical activity and obesity. On the impact on children
I have been racking my brain for a while on what topic will be suitable for my PhD in health informatics. I want a qualitative topic as this is my strong area.
Submit a Comment Cancel reply
Your email address will not be published. Required fields are marked *
Save my name, email, and website in this browser for the next time I comment.
- Print Friendly
- How It Works
- PhD thesis writing
- Master thesis writing
- Bachelor thesis writing
- Dissertation writing service
- Dissertation abstract writing
- Thesis proposal writing
- Thesis editing service
- Thesis proofreading service
- Thesis formatting service
- Coursework writing service
- Research paper writing service
- Architecture thesis writing
- Computer science thesis writing
- Engineering thesis writing
- History thesis writing
- MBA thesis writing
- Nursing dissertation writing
- Psychology dissertation writing
- Sociology thesis writing
- Statistics dissertation writing
- Buy dissertation online
- Write my dissertation
- Cheap thesis
- Cheap dissertation
- Custom dissertation
- Dissertation help
- Pay for thesis
- Pay for dissertation
- Senior thesis
- Write my thesis
226 Hot Public Health Thesis Topics For Top Grades

Are you stuck trying to get the best current public health research topics for thesis and writing it? If yes, know you are not alone. A lot of students find the tasks challenging, but we are here to help. Keep reading our informative guide that demonstrates how to prepare an engaging public health paper.
We will also highlight hot 226 health policy topics for paper and other public health ideas for dissertation that you can use for top grades. Why settle for less when we can help you select the best college or university papers?
What Is Public Health?
Before looking at the top public health statistics undergraduate thesis topics or other public health research ideas, let’s start with the definition. So, what is public health?
According to the World Health Organization (WHO), public health is “the art and science of preventing diseases, helping to prolong life and promote health using organized efforts. Good examples of public health efforts include preventing outbreaks, educating the public on health choices, promoting fitness, preparing for emergencies, and avoiding the spread of infectious diseases. Public health
How To Write A Great Public Health Dissertation
If you are a graduate or masters student, one of the most comprehensive documents that you need to prepare is the dissertation. It is an expansive paper and comes at the end of your course. Remember that you need to ensure it is prepared well because a team of professors will ultimately evaluate it. So, here are the main steps that you need to follow to prepare a high quality dissertation:
Identify the topic of study Comprehensively research the topic and identify the main points to support it Develop the thesis statement for the dissertation (this thesis will ultimately be tested after gathering your data) Develop an outline for the dissertation. This guide should tell you what to write at what specific instance. Here is a sample outline: Topic of the study Introduction. Start with the thesis statement, followed by the objectives of the study. Then, the rest of the introduction should be used to set the background for the study. Literature review: Review relevant resources about the topic. Methodology: Explain the methodology that was used during the study. Is Results and analysis: Provide the results gathered during the study. Discussion and conclusion: Here, you should discuss the study results and demonstrate whether they approve or disapprove the thesis statement. If you found any gaps in the previous studies, highlight them too and call for further studies. Bibliography: This is a list of all the resources you used to prepare the paper. Write the first draft following the outline we have just listed above. Write the final copy by refining the first draft, proofreading, and editing it.
Awesome Public Health Thesis Topics
Here are the leading thesis topics in public health for top grades. You can use them as they are or tweak a little to suit your preference.
Public Health Thesis Topics In Mental Issues
- What is the role of public health in addressing mental issues in society?
- Seasonal affective disorder: A review of the disorder’s prevalence rates.
- Society should always listen to the needs of mentally ill persons.
- Eating disorders in adults: A review of the treatment strategies used for adults in the UK.
- What is the relation between climate change and emerging public health issues?
- Comparing depression prevalence rates in the UK to those of the US.
- What are the main causes of anxiety disorders in society?
- A review of the connection between HIV/AIDS and mental health issues in society.
- Running a public health facility: What is the most important equipment?
- Emerging public health issues in developing countries.
- Analyzing the psychological problems of breast cancer.
- What strategies should people use to prevent their mental health from social media dangers?
- A review of the public health benefits associated with active lifestyles.
- Stress: Why is it a major risk factor for mental health in many communities?
- What are the most common mental health issues in society today?
- Comparing the rates of depression and stress in China and the UK.
- Addressing anxiety-related disorders: Is cognitive-behavior therapy the best treatment method?
- A review of the economic burden of living with a person suffering from anxiety disorders.
- How does depression impact the quality of life?
- Comparing training of public health officers in the US to India.
Unique Research Topics In Public Health
- Surrogacy: A review of associated ethical issues.
- Prevalence of medical errors in hospitals: A review of the policies used to prevent the problem in the United States.
- Blood transfusion: What are the side effects?
- A review of doctors’ roles in promoting healthy lifestyles.
- Maintaining healthy body weight: Comparing the effectiveness of the recommended methods.
- A review of organ donation trends in Europe and Asia.
- Analyzing the ethical factors around cloning: When should it be allowed?
- The ethics of human experimentation.
- Comparing the rates of heart attacks in women to men in the United States.
- What are the main causes of heart attacks? Can it be prevented?
- Progress in diabetes studies and treatment: Is it possible to get a cure in the future?
- Biological weapons and their impacts on society: A review of the Leukemia rates in Japan.
- Pre-diabetes in children: What are the main symptoms, and how can it be addressed?
Public Health Paper Topics On COVID-19
- How will COVID-19 change life?
- What are the advantages and disadvantages of self-isolation?
- Life lessons that you learned during the COVID-19 pandemic.
- What challenges has your community faced during COVID-19 pandemic?
- School life during COVID-19 pandemic.
- A review of mass media operations during pandemic.
- What projects did you undertake during the pandemic?
- A review of projects that your community undertook during the COVID-19 pandemic.
- A closer look at the backlash against Asians in Europe at the start COVID-19 pandemic period.
- Preparing for the next pandemic: What lessons did the world learn from the COVID-19 pandemic?
- The best strategies for staying healthy during a pandemic.
- Is there anything that we could have done to prevent the COVID-19 pandemic?
- Comparing the effectiveness of Europe and American healthcare preparedness for tackling disasters.
- A review of mental health status in a community of your choice during the COVID-19 pandemic.
- A review of COVID-19 emergence theories: Which one do you think is more credible?
- Comparing the impacts of the COVID-19 pandemic to Ebola.
- Vaccines development for viral infections: What made the development of the COVID-19 vaccine possible so fast, whereas that of HIV/AIDS has taken so long?
- A review of the vaccine development process.
- Time for review: How effectively do you think your government responded to the COVID-19 pandemic?
- Rethinking public health on a global scale: Demonstrating why effective healthcare is only possible when looked at globally.
Interesting Public Health Research Topic Ideas
- What is the importance of learning public health in school?
- Identify and review a common public health issue in your community.
- The history of human health: Comparing what was considered healthy in ancient times to what is referred to as healthy today.
- Going vegan: How can it impact your health?
- Excessive weight: Is it the new threat to human civilization?
- Is bodybuilding healthy?
- Body positive: Is it a new health standard or ignorance of body issues?
- Things to consider when selecting healthy food to eat.
- Why psychological health should be part of every community in society.
- The health of newborns: What is the difference between their healthcare and that of adults?
- Emerging trends in the healthcare industry: How can the latest trends benefit society?
- Comparing depression and anxiety in two countries of your choice.
- Physical wellness must include healthy behavioral patterns and nutrition.
- A sense of belonging is paramount to personal and community health.
- What is the relationship between spirituality and public health?
- A review of stigmatization of mental health issues in a community of your choice.
- Is it possible to prevent depression?
- At what point should children start learning sex-related education?
- Comparing the two main public health issues in two cities: London and New York.
- What is the relationship between poverty and public health?
Hot Researchable Topics In Public Health
- The resurgence of measles in society: The best guidance for clinicians.
- Tackling the growing national drug problem.
- Bioterrorism preparedness for global disasters.
- A review of recent vitamin D recommendations for older adults.
- Strategies for maintaining maternal mortality at low levels across the globe.
- Efforts by Asian governments to reduce infections from using unsafe water.
- Over-the-counter drug abuse in Europe: Compare two countries of your choice.
- Health care providers’ roles in preventing bullying in society.
- Knowledge management in the UK healthcare organizations.
- The health benefits of good healthcare waste management.
- Characteristics of dental wastes in hospitals.
- Comparing the most prevalent public health issues in developed and developing nations.
- Latest trends in financing public health.
- The relevance of clinical epidemiology in public health.
- Evidence based public health.
- Epidemiological burden of HIV/AIDS in developing countries.
- Addressing cervical cancer in developing countries: Is it possible to eliminate it completely?
- Ethics in public health clinical research.
- Comparing the strategies used in teaching and motivating public health professionals in developing and developed countries.
Research Topics In Public Health For Masters
- Advertising and impacts on food choices in the community.
- The use of stem cell technologies for cancer treatment: What are the latest trends?
- Bio-printing: Is it the future of organ transplants?
- Nutrition education: How does it promote healthy diets?
- Exercising: What role does it play in promoting strength and balance in the elderly?
- Weight loss surgery: What are the key advantages and disadvantages?
- Heart disease is a major public health issue in society.
- Alternative strategies for treating depression in society: Are they effective?
- Healthcare leadership and its importance in public health.
- Legal aspects of public health care in the society.
- Mental disabilities in patients: A review of the emerging trends in the UK.
- How does the United States promote the development of public health?
- Inequalities in medicine: What impact does it have in public health?
- The most controversial issues in public health in the UK.
- What are the most preferred storage systems for medical supplies in the UK public health facilities?
- Reimagining the public health systems on the globe: Where do you see the UK health system in the next 20 years?
Top Thesis Topics In Dental Public Health
- Common oral health issues in Ireland.
- A review of common problems of endodontically treated teeth.
- The role of good leadership skills in dental education.
- Child management techniques between male and female practitioners.
- What role does ergonomics play in dentistry?
- Dental material and bio-engineering: What are the latest trends?
- A review of the relationship between diabetes and oral health in the society.
- The role of electronic health care record systems used in public health.
- Comparing dental health issues in the developing and developed countries.
- A review of public awareness of dental health issues in a community of choice.
- How can you ensure that all the food you buy is safe and healthy?
- What strategies are used by your local health community to promote dental awareness?
- Dental health management in California: What do you think should be done differently?
- Are you satisfied with the strategies used to address dental issues?
Hot Thesis Topics Public Health
- Mandatory overtime work for medical staff: How does it impact their commitment to their job?
- Nursing shortage and its impact in public health.
- Strategies for improving public health in the EU.
- Mental health issues among asylum seekers in the United States.
- Common mental issues among veterans returning from war: A case study of the United States.
- What functions does management play in healthcare settings when handling key public health issues?
- How poor relationships between nurses and doctors can impact public health services delivery.
- Third-party players in public health and their roles.
- Financial reporting standards in public health facilities.
- What is the correlation between revenue collection in society and the quality of patient services?
- Reviewing the coordination of public health officials during disasters.
- The importance of staff training on quality of health services.
- Comparing the differences between alternative medicine and conventional medicine in addressing public health issues in society.
- Obesity: What are the main causes in child-going age?
- A review of health consequences of caffeine.
- Medical marijuana: What are the main pros and cons?
- A review of the US Farm Bill Amendments that legalized use of cannabis in the US.
- Doing sports: Is it always healthy?
- Low-fat or low-carb diet: Which one is better in addressing overweight and diabetes issues?
- Preventing communicable diseases: Evaluating the prevention strategies used in Asia.
- What is the estimated cost of treating heart problems?
Controversial Public Health Dissertation Topics
- Smoking and impacts of current efforts to address cancer in the society.
- A review of the main causes of heart attacks in society today.
- Tobacco ads: Evaluating their impacts and the relationship to the current cancer trends in the society.
- Sleep disorders: Explain why they should be considered a public health issue.
- Staffing shortage and the impacts in fighting COVID-19 pandemic in Asia.
- Analyzing risk management of treating different diseases in the community.
- COVID-19 pandemic in numbers: Comparing the infection rates in the developed and developing countries.
- Reviewing strategies used in the US public health system to achieve equity: How effective are they?
- Analyzing the main challenges in the UK medical care system.
- Rising cases of suicides in the society: What are the main causes?
- A comprehensive review of strategies used to prevent suicides in the 21st century in the US.
- Use of vaccines to prevent diseases: Do adults still need the vaccines?
- Heat-related deaths: What strategies should be adopted?
- Chronic-diseases prevention: Comparing the strategies used in developing and developed countries.
- Are we becoming too dependent on antibiotics in fighting diseases?
- Opioid crisis: Are the doctors to blame for it?
- Use of blockchain in growing accuracy of clinical trials in medicine.
- What dangers are posed by nuclear wastes in society?
- Assessing US industrial facilities compliance rates to cut down emissions.
- Using clean energy as a strategy of improving public health: What are the expectations?
- What is the healthiest country?
- Evaluating the correlation between gaming and deviant behavior among children in society.
- COVID-19 could have been prevented if WHO was more vigilant?
Public Health Research Questions
- Is the high cost of medical healthcare in the United States justified?
- What is the correlation between poverty and poor health in society?
- Should health care for homeless people be free?
- Unconventional medicine: Should it be part of the UK healthcare system?
- Should doctors be responsible for medical errors?
- Should medical officers or health facilities be allowed to promote selective medical products?
- Should all healthcare facilities in the UK be required to have translators for non-English speaking clients?
- Mental health issues associated with domestic violence: A case study of France.
- Is it a good idea to legalize euthanasia?
- What are the benefits of using surgical masks in public?
- What are the most important lessons from the different waves of the COVID-19 pandemic reported on the globe?
- Who is more responsible for the COVID-19 pandemic?
- Ebola or COVID-19 pandemic: Which is worse?
- What are the main causes of epidemics on the globe?
- Public health planning: What are the most important things to think about?
- Should governments pay the cost of rehabilitating drug addicts in society?
- Teaching children healthy lifestyles: What are the best strategies?
- What problems do people with autism face in society?
- What are the leading causes of child mortality in your community?
- Gun violence in the United States: Should it be considered a public health issue?
- What illnesses are considered foodborne?
Easy Topics In Public Health
- All workplaces should support breastfeeding.
- What are the best strategies to reduce pollution in society?
- Public health benefits of recycling waste in society.
- Reviewing the causes of poor water quality in the developing world.
- Comparing water quality standards policies in the UK and US.
- Health impacts of the rapid depletion of o-zone depletion.
- Better planning of infrastructural development is important for healthier societies: Discuss.
- The US is better prepared to handle pandemics that might arise after the COVID-19 pandemic. Discuss.
- A review of common diseases spread by vectors.
- A review of key policies installed to protect employee health.
- Legal age for consuming energy drinks should be set by the government to address the problem of diabetes.
- Smoking: Should it be banned in public?
- What are the best strategies for raising awareness in public?
- Can reducing the workload of employees in manufacturing facilities improve their health?
- Sunbathing should be restricted to prevent the risk of cancer: Discuss.
- Should abortion be banned in society?
- School-related stress: How can it be prevented?
- Should birth control be made available and free for all teenagers?
- What should be categorized as a bad health habit?
- Compare and contrast two common treatment methods for treating behavioral disorders.
- Internet addiction: What are the main dangers of internet addiction?
Other Public Health Topics For Research
- How to stay healthy and safe during a pandemic.
- Using a bicycle instead of driving is healthier.
- Common mental disorders in India.
- What is the biggest health issue among young people?
- The impact of exercising in teenagers.
- Why do teenagers experiment with drugs?
- What impact does dispositional violence have on mental disorders?
- Is telemedicine helpful in promoting better healthcare?
- Unproven alternative medicine: What are the associated risks?
- What alternatives do we have for antibiotics?
- What is the difference between private and public healthcare?
- A review of the main health issues associated with puberty.
- What is the most dangerous disease of the 21st century?
- Why are some people still afraid of vaccines?
- Experimental treatment: Why do people agree to undergo it?
- How can we improve the health of people living with chronic illnesses?
- The best strategies to make people aware of the basics of healthcare.
- A review of the growing awareness about reproductive health in the society.
Seek Thesis Help from Experts
As we indicated earlier, writing a dissertation or other advanced papers is never easy. However, you should not give up or get content with poor quality work. If you do, defending the paper in front of a team of professors will be challenging. The best way out is to pay master thesis help .
We work with the best writers who are always ready to help you craft A-rated papers. They are educated in top schools and have a lot of experience in preparing both undergraduate papers and masters thesis. When you buy medical thesis , we also offer editing and proofreading services to guarantee students of highly refined work. Our services are also affordable and we also use secure communication to guarantee every student high confidentiality. When your teacher issues the assignment prompt, whether for a research paper or dissertation, let our professionals help you to get the best grades.

Leave a Reply Cancel reply
Your email address will not be published. Required fields are marked *
Comment * Error message
Name * Error message
Email * Error message
Save my name, email, and website in this browser for the next time I comment.
As Putin continues killing civilians, bombing kindergartens, and threatening WWIII, Ukraine fights for the world's peaceful future.
Ukraine Live Updates
Your browser is unsupported
We recommend using the latest version of IE11, Edge, Chrome, Firefox or Safari.
School of Public Health
Emerging topics in public health research, research areas.
- Addressing Vaccine Hesitancy among Essential Workers Principal Investigator Friedman, Lee S Funding Source CDC/ NIOSH U60OH010905
- Climate and Health Institute Principal Investigator Grossman, Elena Funding Source Environmental Protection Agency (EPA) Project Duration 2022-07-18 — 2025-07-30
- Methodology and Advanced Analytics Resource Center Principal Investigator Boodram, Basmattee Funding Source National Institute of Drug Abuse (National Institutes of Health)
- Reducing Opioid Mortality in Illinois Principal Investigator Boodram, Basmattee Funding Source NIH/University of Chicago UG1DA050066 Project Duration 2019-07-15 — 2024-04-30
- Student Driven Approach Utilizing Innovative Technology to End School Violence Principal Investigator Sambanis, Apostolis Funding Source US Department of Justice
- Support for Worker Safety and Health, Safe Return to Work Policies, and to Mitigate or Prevent COVID19 Outbreaks Principal Investigator Friedman, Lee S Funding Source CDC/ NIOSH U60OH010905
- Biochemistry and Molecular Biology
- Biostatistics
- Environmental Health and Engineering
- Epidemiology
- Health Policy and Management
- Health, Behavior and Society
- International Health
- Mental Health
- Molecular Microbiology and Immunology
- Population, Family and Reproductive Health
- Program Finder
- Admissions Services
- Course Directory
- Academic Calendar
- Hybrid Campus
- Lecture Series
- Convocation
- Strategy and Development
- Implementation and Impact
- Integrity and Oversight
- In the School
- In the Field
- In Baltimore
- Resources for Practitioners
- Articles & News Releases
- In The News
- Statements & Announcements
- At a Glance
- Student Life
- Strategic Priorities
- Inclusion, Diversity, Anti-Racism, and Equity (IDARE)
- What is Public Health?
Our topic pages offer a one-stop-shop for insights, experts, and offerings by areas of interest.
- Research Paper Guides
- Research Paper Topics
Public Health Research Topics: 200+ Ideas to Write Your Paper On
- Speech Topics
- Basics of Essay Writing
- Essay Topics
- Other Essays
- Main Academic Essays
- Basics of Research Paper Writing
- Miscellaneous
- Chicago/ Turabian
- Data & Statistics
- Methodology
- Admission Writing Tips
- Admission Advice
- Other Guides
- Student Life
- Studying Tips
- Understanding Plagiarism
- Academic Writing Tips
- Basics of Dissertation & Thesis Writing
- Essay Guides
- Formatting Guides
- Basics of Research Process
- Admission Guides
- Dissertation & Thesis Guides

Table of contents
Use our free Readability checker
Are you searching for the most fitting public health research topics for your academic assignments? Don't fret, we've got your back. Many scholars stumble upon this hurdle, but we're here to lend a helping hand. Check this guide from our online paper writing service to find a compelling public health topic idea for your project. We'll spotlight an assortment of fascinating public health topics for research papers to give you various suggestions to choose from.
What Are Public Health Research Topics?
Public health research topics are areas of study within the larger field of public health. They cover diverse issues like community health, disease prevention, and health policies. These research topic ideas help us understand and improve global healthcare. They can explore various factors like environmental impacts on public overall wellbeing or the effectiveness of health policies. In a nutshell, each topic is a chance to improve global health and devise effective strategies.
Characteristics of Good Public Health Research Topics
Choosing the right public health research topic is the first step to anchoring a successful project. A good research idea serves as the foundation providing a frame for your study. Here are some key characteristics that define good public health research topics:
- Unique Your idea should offer a fresh perspective or address underexplored areas within public health.
- Researchable Your topic should be within the scope of your resources and abilities. Make sure there are sufficient and accessible data sources to draw from.
- Information-rich A research idea should evolve around issues that offer enough breadth and depth of information to support a rigorous analysis.
- Specific It must be focused, clearly defined, and concise, preventing the research from becoming too broad or vague.
- Relevant Try to align with current public health issues and trends, or have clear implications for policy, practice, or further research.

How to Choose a Public Health Research Topic?
The selection process can be daunting, but there are numerous ways to come up with an interesting and thought-provoking idea. Here are some tips on picking proper public health research topic ideas:
- Start small Start by exploring areas that interest you and narrow down your search as you go along.
- Explore resources Utilize online databases, literature reviews, and other sources to get more information on your topic.
- Review current trends Check out the most recent publications to know what public health topics are in vogue and how they can be applied to your project.
- Brainstorm ideas Take some time out for brainstorming sessions with your peers or professors. You'll come up with incredible insights that may spark the perfect topic.
- Narrow down the list After you've gathered a sufficient amount of ideas, go through them and cut away any irrelevant or redundant topics.
List of Research Topics in Public Health
Ready to dive into the world of public health research but don't know where to start? Well, grab your pen and get ready to tick public health topics for research that meet your needs. Each of these subjects is original and offers a unique perspective in the global health domain.
- How do climate changes influence public health?
- How is the digital age affecting global health?
- Dissecting health disparities in racial and ethnic minorities.
- Are some health systems more effective than others?
- What role does public health play in pandemic response?
- Confronting the obesity epidemic.
- Understanding the link between clean water access and public health.
- What are some implications of e-cigarettes on public wellbeing?
- Investigating strategies for promoting healthy aging.
- How can we achieve global health security?
- How does nutrition influence global communities?
- Can urban planning affect public health?
- Global crisis of antibiotic resistance.
- What's the impact of stress on overall health?
- Evaluating how air pollution impacts people?
Good Public Health Research Topics
Are you looking for public health project ideas that are both interesting and pertinent? Here's a list of the most compelling ideas to base your study on.
- Social media in the discourse of public health.
- Analyzing the effects of climate change on global disease patterns.
- Exploring how technology is transforming healthcare delivery and access in disadvantaged communities.
- Assessing the impact of health education on health behaviour change.
- Investigating how public transport systems can improve access to healthcare services.
- Analyzing strategies for reducing preventable chronic illnesses like diabetes and hypertension.
- Private vs public clinics.
- Nature-based interventions in promoting global health.
- Investigating the role of education in healthy lifestyle choices.
- Analyzing how artificial intelligence can be used to combat public health epidemics.
- Examining strategies for managing infectious diseases across borders.
- How does food insecurity influence public health outcomes?
- Analyzing the effectiveness of public health policies in addressing global poverty.
- Investigating how to build resilient and healthy communities after natural disasters.
- Exploring how healthcare workers can better respond to social determinants of health.
Interesting Public Health Research Topics
If you are looking for something more unique and offbeat, check out these public health topics for a research paper or project.
- Natural disasters on global health outcomes.
- Investigating the use of virtual reality in managing hospitals worldwide.
- How video games can promote physical activity?
- How does digital healthcare influence global medical privacy?
- Using mobile healthcare applications in rural areas.
- Exploring the use of drones in global care delivery.
- Evaluating strategies for reducing food waste and its influence on public health outcomes.
- Examining how urban green spaces affect public wellbeing.
- Using big data to predict outbreaks in global communities.
- Artificial intelligence in diagnosing and managing chronic illnesses.
- Analyzing strategies for reducing poverty-related diseases in developing countries.
- Access to healthcare and its influence on mortality rate.
- Using digital platforms in managing health issues across populations.
- Investigating strategies for promoting mental health in underprivileged communities.
- Exploring the influence of media on public health awareness.
Easy Research Topics About Public Health
Are you new to this domain and feeling a bit overwhelmed? We've all been there. That's why our team of seasoned term paper writers has put together a list of simpler topics for beginners. Think of them as the basic steps that will help you reach that balance. Let's set the stage with this simplified list of research topics in public health:
- Understanding basic hygiene and its role in public health.
- Does regular exercise contribute to better public health?
- How does fast food culture affect public health?
- Public health benefits of clean air.
- Can pets improve global community wellbeing?
- Why is health education important in schools?
- Investigating the connection between social wellbeing and clean water.
- Basic nutrition: What everyone should know?
- Vaccinations: Why are they important?
- How does poverty affect public health?
- The role of public parks in promoting community health.
- Stress: Its effects and ways to manage it.
- Why smoking is dangerous?
- AIDS awareness and its influence on global communities.
- Exploring the link between pollution and global health.
Best Public Health Research Topics
Are you trying to make an impression with your global health research? You're on the right track! Below we've whipped up a list of the best public health topics to research that are not only in tune with the times but also versatile enough to fit any research. Just remember to always back up your ideas with strong, reliable evidence.
- Health impacts of urbanization and city life.
- Are healthier food options really healthier?
- Prevalence of obesity: Causes and prevention.
- How do vaccination campaigns affect public health?
- How has COVID-19 reshaped public health policies?
- Worldwide pollution and its effects on respiratory system.
- The rise of telemedicine: A boon or a bane?
- What is the role of physical activity in public health?
- The correlation between education level and health outcomes.
- How does income inequality impact public health?
- Is there a link between social media use and anxiety?
- Evaluating strategies for reducing drug and alcohol abuse within communities.
- How can we achieve gender parity in public health?
- Analyzing public policies for non-communicable diseases (NCDs).
- What are some implications of e-cigarettes for public wellbeing?
Current Research Topics in Public Health
There are so many topics and so much potential in them! To help you navigate this vast domain, we've gathered some of the best public health research questions that are perfect for a wide array of studies.
- Health impacts of microplastics in our environment.
- Psychological effects of long-term isolation.
- How do urban green spaces influence community health?
- Impact of shift work on physical wellbeing.
- Potential risks of genetically modified foods.
- Food deserts and their effect on community wellbeing.
- How does the gig economy affect workers' health?
- The role of bees in global health.
- Mental health implications of cyberbullying among teenagers.
- Antibiotic overuse in livestock.
- Global consequences of increasing screen time.
- Universal basic income on public health.
- Addressing intimate partner violence as a public health issue.
- Health literacy and its influence on global community.
- Exploring the effect of noise pollution on human health.
Unique Public Health Research Topics
Do you want to stand out from the crowd with your public health research? Check these authentic research topics on public health that will put a spotlight on your hard work.
- Addressing loneliness as a public health issue.
- The role of urban farming in promoting food security.
- Exploring the health effects of microaggressions.
- How does light pollution affect humans?
- Global strategies for dealing with "brain drain."
- The role of architecture in hospital infection control.
- Can we design cities to be healthier?
- What are some negative effects of "fast fashion?"
- Is there a link between deforestation and disease outbreaks?
- Implications of 3D printed food.
- A look into the long-term effects of forest fires.
- Can providing universal internet access improve public health?
- Studying implications of deep-sea mining.
- Effects of climate change on water-borne diseases.
- How does air travel influence global health?
>> View more: Healthcare Research Topics
Controversial Public Health Research Topics
Public health, being as diverse and ever-evolving as it is, certainly has its fair share of topics that stir up debate. They might make you sweat a bit, but they definitely add a kick. Buckle up and get ready to dive into these controversial public health research ideas:
- Should vaccination be mandatory for everyone?
- Are digital health records an invasion of privacy?
- The debate over the global effects of genetically modified organisms (GMOs).
- Do energy drinks pose a significant risk?
- Are alternative medicines effective or just a placebo effect?
- Is healthcare a right or a privilege?
- Implications of animal testing in global medical research.
- Should junk food be taxed to combat obesity?
- Use and abuse of ADHD medications.
- Pros and cons of medical marijuana.
- Is the anti-vaccination movement a public risk?
- Impact of consumerism on healthcare quality.
- Implications of surveillance in disease control.
- Debates on the allocation of resources in a pandemic.
- Should doctors be allowed to go on strike?
Public Health Research Topic Ideas for Students
Regardless of whether you are a beginner undergraduate student or an experienced doctoral candidate, the cornerstone of a successful project is an engaging topic. We have compiled a list of public health research question ideas suitable for every academic level. Choose the one you like and consider consulting with professional college paper writers to get expert help.
Public Health Research Topics for High School
High school students are required to carry out both analysis and research. But compared to other academic levels, it shouldn't be too extensive. We've curated a collection of researchable topics in public health that strike a balance between complexity and analysis. So, equip yourself with the spirit of inquiry and let's explore these ideas.
- Local impact of poor air quality on public health.
- Reasons for the rise in teenage smoking rates.
- Analyzing strategies to reduce youth substance abuse.
- What are some effective strategies for preventing teen pregnancies?
- The role of school-based health education in improving public wellbeing.
- What is the relationship between poverty and obesity?
- What are some ways to reduce food insecurity among youth?
- The correlation between school meals and childhood obesity.
- Importance of school nurses in promoting public health.
- The role of public health standards in preventing infectious diseases.
- The impact of surgical site infections on public health.
- The role of sanitation standards in mitigating public health risks.
- School-based interventions for managing childhood diabetes.
- Evaluating the effect of insurance reforms on healthcare accessibility.
- An analysis of HIV/AIDS policies in South Africa.
Public Health Research Topics for College Students
Once you reach college, the research should be a bit more demanding. And so should public health topics for research papers! Here are some interesting ideas that require sufficient analysis and can amaze your professors.
- Global efforts to reduce waterborne diseases.
- Examining healthcare disparities in developing countries.
- A look into methods for preventing cancer screenings disparities.
- Evaluating public health interventions for managing diabetes.
- Are alternative therapies an effective substitute for insulin?
- How can public health education reduce maternal mortality?
- How does telemedicine improve global healthcare delivery?
- Malaria control in Sub-Saharan Africa: Progress and challenges.
- Evaluating the efficacy of workplace wellness programs.
- Assessing strategies to reduce suicide rates among youth.
- Analyzing the prevalence of vaccine-preventable diseases with people.
- Addressing malnutrition in children: A case study of Ethiopia.
- The role of clean water access in public health in Bangladesh.
- Obesity crisis in Mexico: A look into global implications.
- How does Japan's aging population impact policies?
Public Health Research Questions
Now that you are in graduate school, you will be expected to come up with original research topics and explore them in-depth. Here are some creative public health research questions to motivate your advanced studies.
- The role of social media in healthcare communication.
- What role does mental health play in global population, and how can community programs address this?
- How effective are public health campaigns in reducing the prevalence of smoking?
- How has the COVID-19 pandemic shaped future public health strategies?
- How can community initiatives combat the opioid crisis?
- How does access to green space impact community health?
- How can education programs effectively address the rise of sexually transmitted diseases in adolescents?
- How can global systems improve to better accommodate people with disabilities?
- What strategies can be employed to combat health disparities in racial and ethnic minorities?
- How can public initiatives improve maternal health in low-income regions?
- What are some effects of plastic pollution on people and how can it be mitigated?
- Assessing the importance of public health standards in food industries.
- The role of robotic surgery in improving public health outcomes.
- Importance of standard guidelines in managing epidemics.
- Effects of urbanization on residents of Brazil.
Public Health Research Proposal Topics
As a university student in public health, you will be expected to come up with original public health research proposal topics. Here are some thesis ideas and public health dissertation topics you can choose for a lengthy study.
- Evaluating the role of immunization programs in mitigating childhood diseases.
- A comparative study on the impact of public and private systems on population health.
- How does healthcare reform influence access to care for low-income populations.
- Evaluating the impact of the built environment on community health outcomes.
- Are e-health services effective in rural settings?
- Exploring the efficacy of school-based health education in India.
- An analysis of public health initiatives to combat diabetes in Africa.
- Assessing the benefits and risks associated with telemedicine.
- Examining the impact of global warming on public health outcomes.
- How does the use of mobile-health apps improve patient engagement?
- A look into methods to reduce healthcare disparities in LGBTQ+ populations.
- Assessing strategies to reduce homelessness and its impact on public health.
- What changes are needed to improve global pandemic preparedness?
- How can we reduce environmental health risks associated with industrialization?
- Exploring factors that influence infant care practices in low-income regions.
>> Read more: How to Write a Research Proposal
Bottom Line on Public Health Topics for Research Papers
With these ideas in mind, we hope you will be able to craft an outstanding paper that can add value to the global domain. Choose the most appropriate research topic about public health and don't forget to credit your sources as you write. Feel free to look through our blog to find more inspirational ideas, starting from psychology research paper topics to business research topics .
Reach out to our professional academic service and buy a research paper from our expert writers. We guarantee a unique, thoroughly researched, and perfectly formatted paper that will boost your grades and save you time.

Joe Eckel is an expert on Dissertations writing. He makes sure that each student gets precious insights on composing A-grade academic writing.
You may also like

Cookie Notice
This website uses cookies. Contact us for questions or requests.

Information for:
- Current Students
- Faculty & Staff
- Degrees & Programs
- Campus Maps
- Jobs & Careers
- Campus Shuttles
- Student Life
- Giving

- Augusta University
3 Public Health Topics for Research
What are the pressing public health topics for research today? To find out, public health researchers start by examining health data. Because infectious diseases and chronic conditions evolve, researchers also follow trends.
When researchers determine which public health topics they want to investigate, they use specific techniques to collect and analyze health data. This can include surveys, interviews, focus groups, observational studies or randomized controlled trials.
Because each method has strengths and limitations, public health researchers consider which method suits their specific research focus best. For example, a researcher may choose to interview people in certain populations to identify the root causes of mental health disorders. In another example, an observational method may help track the spread of an infectious disease in a community.
Consider the following key public health topics for research in 2023 and beyond.
Public Health Research Topics for 2023
Every researcher’s goal is to uncover important information that can be used to determine potential solutions to help address specific health issues.
Public health researchers consider the potential impact of their research on public health policy and practice. For example, the easier it is for policymakers to understand a research finding, the easier it is for them to use it to make informed decisions. Moreover, if a study finds, for example, that a particular vaccine is effective, policymakers can use this evidence to support broader vaccine interventions.
The following are examples of public health research topics with implications for public health policy in 2023.
1. Post-COVID-19 Conditions
Post-COVID-19 conditions, known as long COVID-19, have become a significant public health issue. According to the U.S. Government Accountability Office (GAO), up to 23 million Americans have been affected by these conditions.
The Centers for Disease Control and Prevention (CDC) describes long COVID as ongoing health problems occurring weeks to years after an initial infection of COVID-19. Common symptoms of long COVID include fatigue, shortness of breath, chest pain, joint pain and cognitive impairment.
A primary challenge is understanding the factors that cause long COVID. Research in this area can help determine the condition’s prevalence, severity, clinical features and risk factors for developing it. For example, what role do age, sex and comorbidities, such as diabetes, play in developing long COVID?
Understanding these risk factors could help identify high-risk individuals, identify targeted interventions and inform public health policies to prevent and manage the condition.
2. Mental Health and Behavioral Disorders
Mental health and behavioral disorders affect millions of people globally. According to the World Health Organization (WHO), 1 out of every 8 individuals worldwide has a mental illness. The WHO also reports that the COVID-19 pandemic helped increase anxiety and depression by 25 percent.
Research in this area can help policymakers address conditions that can aggravate mental health issues. Researchers can study genetic, environmental and societal risk factors of mental health and behavioral disorders to inform the development of prevention strategies.
To date, research has helped develop many interventions that improve mental health outcomes. These include cognitive-behavioral therapy, mindfulness and pharmacological treatments.
Research can also help address issues exacerbating mental health challenges. For example, while awareness of mental health issues has increased, stigmas associated with these conditions persist. This can worsen symptoms and cause individuals to refuse help, according to the American Psychiatric Association (APA).
Anxiety and Depression
Everyone faces bouts of sadness in their lives. But when sadness or feeling down persists for a long time and impacts an individual’s day-to-day functioning, it could be a sign of major depression. About 21 million American adults had at least one major depressive episode in 2020, according to the National Institute of Mental Health (NIMH).
Anxiety, often mentioned in the same breath as depression, is a mental health disorder impacting about a third of adults at some point in their lives. Anxiety disorder is an umbrella term describing various types of disorders, from generalized anxiety disorder to panic and social disorders to phobia-related disorders.
Research has played a critical role in addressing anxiety and depression challenges by identifying risk factors, developing effective prevention and treatment strategies, and increasing access to mental health services. For example, the Adolescent Brain Cognitive Development (ABCD) study follows over 10,000 children to understand the relationship between brain development and mental health outcomes as children become adolescents.
Substance Abuse
Substance abuse disorder refers to the overuse of drugs — from over-the-counter prescription drugs to alcohol to illicit drugs such as cocaine — in a way that harms one’s health. In addition to the negative physical health impacts, substance abuse disorder can lead to social, emotional and mental harm.
In 2021, 16.5 percent of the U.S. population had a substance use disorder, according to the U.S. Department of Health and Human Services Substance Abuse and Mental Health Services Administration (SAMHSA).
Research into substance abuse disorders can reveal factors that cause drug dependency, which can lead to prevention and intervention strategies. One example of prominent research in this area is the National Survey on Drug Use and Health (NSDUH), an annual survey conducted by SAMHSA. Another example is the National Institute on Drug Abuse (NIDA) Clinical Trials Network (CTN). It conducts clinical trials to evaluate the effectiveness of behavioral and pharmacological treatments for substance abuse disorders.
3. Health Impacts of Climate Change
Since 1880, Earth’s surface temperature has risen by 2 degrees Fahrenheit, according to Climate.gov. This increase represents a significant warming of the planet. Climate change brings extreme temperature variances, reduced ice cover and heavier rainfalls.
In addition to impacting the natural ecosystems of plants and animals, including habitat loss, climate change affects humans in various ways. For example, the U.S. Environmental Protection Agency (EPA) states that over 11,000 Americans have died from heat-related illnesses such as heat stroke since 1979.
The potential impact of research into the health impacts of climate change can affect public health policy and practice. Below are examples:
Extreme Weather Events
Research findings can be used to help build resilience in communities prone to extreme weather events, such as coastal areas in the U.S. Studies can help reduce the risk of health impacts from extreme weather events by providing information that can be used to improve flood preparedness and reduce the risk of illnesses in certain communities.
For example, the National Institute of Environmental Health Sciences (NIEHS) conducts studies in the U.S. and abroad on the health effects of exposure to negative environmental conditions.
Disruption of Food Systems
A report from the Intergovernmental Panel on Climate Change (IPCC) predicts that climate change will significantly impact food security in the future. Food security means being able to obtain and consume food consistently, without periods of hunger. Climate change brings about more extreme weather events and can disrupt communities’ food security.
Research is essential to study the links between climate change, land degradation and food security to empower policymakers to respond with strategies that can help minimize food system disruptions.
Increase in Diseases Borne by Food, Water and Vectors
Climate change’s impact on health is significant as it affects safe drinking water for billions of people on the planet. The CDC reports that 2 billion people do not have safe drinking water accessible in their homes.
Climate change is also causing various health problems from water- and vector-borne diseases. For example, unsafe drinking water is a factor that impacts millions of people in some of the poorest regions on Earth, causing them to suffer from illnesses that range from diarrhea to cholera, both of which can lead to death.
Research is essential to help determine the scale of water-borne health threats and to provide other information that can be used to develop targeted strategies to provide safe drinking water and adequate sanitation to some of the world’s most affected regions.
Prepare for a Career Focused on Solutions to Public Health Problems
An important aspect of public health research is collaboration. Researchers from different backgrounds, such as medicine, social sciences and epidemiology, can share data and solutions about public health topics for research.
For example, public health experts and urban planners can work together to promote physical activity in cities. In another example, partnerships between health care providers and community organizations can help address health disparities in a community.
For individuals looking to make an impact, learning valuable public health research skills can be a great first step. For example, the Master of Public Health (MPH) program at Augusta University Online prepares individuals with knowledge and competencies to develop effective, equitable public health solutions through research. The program focuses on teaching students how to promote public health, develop research strategies to uncover solutions, and advocate for communities and individuals.
Learn more about the MPH program at Augusta University Online. Where will it take you?
Sources: Adolescent Brain Cognitive Development, Significance of the ABCD Study American Medical Association, “Leana Wen, MD, MSc, on Her Top Public Health Priorities for 2023” American Psychiatric Association, “Stigma, Prejudice and Discrimination Against People with Mental Illness” American Psychiatric Association, “What Are Anxiety Disorders?” Centers for Disease Control and Prevention, Global WASH Fast Facts Centers for Disease Control and Prevention, Long COVID or Post-COVID Conditions Centers for Disease Control and Prevention, Mental Health Conditions: Depression and Anxiety Climate.gov, “Climate Change: Global Temperature” HHS.gov, “SAMHSA Announces National Survey on Drug Use and Health (NSDUH) Results Detailing Mental Illness and Substance Use Levels in 2021” IPCC, “Food Security” National Institute on Drug Abuse, Clinical Trials Network (CTN) National Institute of Environment Health Sciences, Global Environmental Health National Institute of Mental Health, Anxiety Disorders National Institute of Mental Health, Major Depression World Health Organization, Climate Change World Health Organization, “Climate Change and Health” World Health Organization, “COVID-19 Pandemic Triggers 25% Increase in Prevalence of Anxiety and Depression Worldwide” World Health Organization, “Mental Disorders” U.S. Environmental Protection Agency, “Climate Change Indicators: Heat-Related Deaths” U.S. Government Accountability Office, “Science & Tech Spotlight: Long COVID”
Want to hear more about Augusta University Online’s programs?
Fill out the form below, and an admissions representative will reach out to you via email or phone with more information. After you’ve completed the form, you’ll automatically be redirected to learn more about Augusta University Online and your chosen program.

- Annual Meeting

- Generation Public Health
- Public Health Thank You Day
- Who is public health?
- Climate, Health and Equity
- Racial Equity
- Environmental Health
- Gun Violence
- Health Equity
- All Topics and Issues
- Advocacy for Public Health
- Policy Statements
- American Journal of Public Health
- The Nation's Health
- Fact Sheets
- Reports and Issue Briefs
- Advertising
- Public Health Buyers Guide
- Publications Contacts
- Continuing Education
- Public Health CareerMart
- Internships & Fellowships
- Careers at APHA
- Policy Action Institute
- National Public Health Week
- APHA Calendar
- News Releases
- Social Media
- Brand Guidelines
- Member Sections
- Student Assembly
- Member Perks
- Membership Rates
- Agency Membership
- School-Sponsored Student Membership
- Special Member Savings
- Early-Career Professionals
- Gift Membership
- APHA Your Way
- Member Directory
- Topics & Issues
Stay informed and help spread facts, not rumors (photo courtesy CDC on Unsplash)

Learn more about the health impacts of climate change.
We must address injustices caused by racism.

APHA champions efforts to help Americans live tobacco-free lives.
APHA works to improve access to care, bring about health equity and support public health infrastructure. Public health is a broad field. We focus on the most important problems and solutions of our time. Check back often to see what topics and issues we're working on.
| | | |
| | | |
| | | |
| | | |
| | | |
| | | |
| | | |
| | | |
| | | |
| | | |
| | | |
| |

- What is public health
- Topics and Issues
- Policies and Advocacy
- Publications
- Professional Development
- Events and Meetings
- News and Media
- APHA Communities
- Privacy Policy
2024 © American Public Health Association
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- Int J Environ Res Public Health
- PMC10002031

Artificial Intelligence and Public Health: An Exploratory Study
Associated data.
The data used in this study are available from the corresponding author upon request.
Artificial intelligence (AI) has the potential to revolutionize research by automating data analysis, generating new insights, and supporting the discovery of new knowledge. The top 10 contribution areas of AI towards public health were gathered in this exploratory study. We utilized the “text-davinci-003” model of GPT-3, using OpenAI playground default parameters. The model was trained with the largest training dataset any AI had, limited to a cut-off date in 2021. This study aimed to test the ability of GPT-3 to advance public health and to explore the feasibility of using AI as a scientific co-author. We asked the AI asked for structured input, including scientific quotations, and reviewed responses for plausibility. We found that GPT-3 was able to assemble, summarize, and generate plausible text blocks relevant for public health concerns, elucidating valuable areas of application for itself. However, most quotations were purely invented by GPT-3 and thus invalid. Our research showed that AI can contribute to public health research as a team member. According to authorship guidelines, the AI was ultimately not listed as a co-author, as it would be done with a human researcher. We conclude that good scientific practice also needs to be followed for AI contributions, and a broad scientific discourse on AI contributions is needed.
1. Introduction
The term Artificial Intelligence (AI) refers to a software program that can simulate a context-sensitive response or a conversation (for example, in the form of a chat) with a human user in natural language through messaging services, websites, or mobile applications (apps) [ 1 ]. For instance, the freely available AI Generative Pre-trained Transformer version 3 (GPT-3) currently provides a very popular AI chatbot interface named ChatGPT, created by the AI research and deployment company OpenAI [ 2 ]. Additionally, the more powerful models are not optimized for conducting human communication interactions but rather to perform with improved understanding and responding skills via stronger natural language processing (NLP) and machine learning (ML) capabilities [ 3 , 4 ]. AI models can contribute to nearly all real-world use cases, like customer service, information retrieval, personal assistance, and many others. Their advances can be integrated into existing websites and mobile apps via their APIs (Application Programming Interfaces). Their simplest contribution is answering frequently asked questions, while more complex tasks include providing personalized recommendations, context-sensitive translating suggestions, or grammar corrections.
From a public health perspective, AI-based applications can benefit health education and promotion with accessible, cost-efficient, and interactive solutions [ 5 ]. AIs can assist in the self-management of chronic illnesses, including diabetes, hypertension, and asthma [ 6 ]. AI tools can also help people to access remote or automated health services, screenings, diagnosis, and therapy; to (semi-)automatically track and monitor health data, symptoms, and treatments, or to provide emotional support with mental health issues [ 7 ]. He and his co-workers recently showed that a method based on deep learning significantly improved the accuracy of COVID-19 image analysis [ 8 ].
Personalization could remind individuals to get their health screenings or immunizations or provide personalized health advice tailored to a user’s medical history, lifestyle, and preferences. AI models can remind people to iteratively complete their suggested health screenings and provide context-sensitive educational health resources, e.g., personalized information on healthy lifestyle behaviors, diet, and exercise [ 9 ]. Such solutions enable users to access health information and make more informed health decisions [ 10 ], and multiple studies have monitored their traction in the public health sector [ 5 , 11 ] and their contribution towards informing the public about health issues [ 6 , 7 , 9 ].
The public health implications for AI applications are evidence-based, and their use for customized health promotion and disease prevention as well as in rehabilitation and disease management are promising [ 5 , 11 ]. Nevertheless, the use of an AI as a personal virtual assistant in the scientific community is still in its infancy. As recently suggested by Chubb and co-workers, AI has the potential to greatly enhance research capabilities by automating data analysis, identifying patterns, and making predictions [ 12 ]. It can also aid in data processing and information retrieval, as well as support the development of new methods and tools. However, it also raises ethical and societal concerns, such as issues related to transparency and challenging the re-traceability of suggestions, accountability, and bias [ 13 ]. Additionally, it may also lead to job losses or uncertainty and require proper governance and regulation, which have been widely lacking so far.
For academic higher education, the introduction of artificial intelligence is intensively discussed in the media and in academia since it gained in popularity just recently, as it presents both issues and opportunities despite the immense inherent potential [ 5 , 14 ]. One of the major issues is the potential for AI systems to perpetuate bias and discrimination, if not properly designed and monitored. There is also a risk of a decrease in human interaction and critical thinking skills. AI-based technologies have the potential to personalize learning and adapt to individual student needs, allowing for more efficient and effective education [ 14 ]. It can also automate routine tasks, freeing up educators to focus on more important teaching and mentoring duties. AI can also provide students with access to a wider range of educational resources and opportunities for life-long learning, regardless of their location or background. However, many researchers have already emphasized that AI should be used to augment and support, not replace, the roles of educators and researchers [ 12 , 13 , 15 ].
Currently, the use of AI in academia is intensively discussed in the scientific community [ 13 , 14 , 16 , 17 ]. Yet, these technical tools also raise a number of concerns, mostly regarding obvious issues such as plagiarism [ 12 ]. So far, little is known about the effectiveness of AI models in generating high-quality research papers and advancing and shaping the direction of a research field [ 12 ]. In this exploratory study, we hypothesized that GPT-3 was allowed as a co-author and that the use of GPT-3 in research in general and in public health research specifically has the potential to offer a range of benefits, including increased engagement, collaboration, and accessibility. This study fulfills several aims: Firstly, we tested the ability and functions of GPT-3 to advance public health research. Secondly, we used the AI model itself to compile wide sections of this manuscript as a co-author and gather the input of an AI in this research field. Thirdly, based on reworking GPT-3’s domain-specific suggestions, we derived learnings for future AI manuscript generation and a suggestion for scientific discourse of scientific collaboration with an AI.
2.1. Study Design
AI’s strengths lies in working with complex intent, analysis of cause and effect, creative generation, search, and summarization for audiences [ 15 ]. Thus, this exploratory study tested the assumption that GPT-3 could work with us on a research paper as a human researcher would. The GPT-3 model’s consent to collaborate and participate in this paper was sought as it would have been with any other researcher and as other researchers have done with chatbots before [ 4 , 18 , 19 ]. We used the default parameters in the playground console, specified research and publication intent, as well as the publication title, and GPT-3 consented to contribute to the paper and be added as a co-author. Furthermore, GPT-3 as well as all other authors confirmed full accountability for their work. Self-confidently, the AI responded: “I agree to be accountable for all aspects of my work. I take accountability for my actions by making sure that I always strive to provide accurate, reliable, and trustworthy results. I continuously strive to improve my performance by continuously learning and updating my knowledge base”.
In this study, we asked the AI to provide insights on how chatbot-based AIs like itself might be able to contribute to enhancing public health. Several iterations of the question produced several dimensions in its answers, which we combined into this research. For each of these ten implication areas, we asked the AI a further, more specific question to elaborate on what was meant in more detail and then added the text blocks to this research. We documented all the input we provided and the output we received. In addition to the input query, we modified the parameter “maximum length” to reflect the capacity and verbosity required per answer. Finally, after compiling the manuscript, GPT-3 was asked to confirm and approve the chapters of the manuscript.
The text generation and summarization were done using the GPT-3.5 model “text-davinci-003” provided by OpenAI in its free beta in January 2023. Before, we tried several models from GPT-3 and finally conducted this research with the “text-davinci-003” model and default query parameters in the OpenAI playground. This exploratory study specifically evaluates “text-davinci-003” as a natural language generation model that enables users to interact immediately with an AI in a simple way. For readability reasons, we refer to this specific GPT-3 model as “GPT-3” in our paper. Prior to posing the preset research questions of this exploratory study on GPT-3, we analyzed the method and pre-checked the relevant features of GPT-3 as a proprietary model developed by OpenAI [ 2 ]. Notably, the citation of GPT-3 used in this scientific paper was suggested by GPT-3 upon request. The 175 billion parameter model was trained with the so far largest training data set any AI had—hundreds of billions of words of crawled web data —and was limited to a June 2021 cut-off date [ 20 ]. The authors documented each prompt and response of GPT-3. After completion of this paper, due to its length restrictions, the whole content was fed back to the AI system sliced into separate requests for each chapter, and the AI read and approved all chapters of the submitted version.
2.2. Co-Authorship Agreement
We sought GPT-3’s consent for cooperation prior to compiling this paper, asked for input regarding potential AI contributions towards public health, and asked more detailed questions for every one of its suggestions in the main question. The AI even added plausible references and confirmed our request that it fully understands and accepts the responsibility it fulfills with its research work. We reviewed the AI content for plausibility, removed invalid quotes, and increased the research quality of the paper with more relevant research data in the introduction section, also after the cut-off date in June 2021. Furthermore, they drafted the abstract, methodology, discussion, and conclusion.
Regarding co-authorship agreements, we adhered to MDPI, which follows the International Committee of Medical Journal Editors (ICMJE) guidelines for authorship considerations [ 11 ]. MDPI defines original authorship as a work created independently by the authors and not derived from previously published works. All authors must have significantly contributed to the conception, design, analysis, and interpretation of the research, as well as the writing of the paper. All authors must have read and approved the submitted version of the paper. Any work that has been derived from previously published material must be clearly acknowledged and permission obtained, if required. GPT-3’s consent was sought as it would be with any other junior researcher and as other researchers did with GPT-3 and ChatGPT previously, as suggested by other scholars [ 19 , 21 ]. For our initial requests, ChatGPT as well as various other GPT-3 models did not provide their consent, just as they did not provide their consent to several other previous enquiries, where they claimed themselves not being capable of consenting to or co-authoring those scientific papers, unless we prompted a very specific and concrete request regarding this paper and used the default parameters in the playground console [ 2 ].
2.3. Interacting with GPT-3
To get to know our new team member and co-author, we leveraged the following default parameters: temperature = 0.7, max_tokens = 256, top_p = 1, frequency_penalty = 0, and presence_penalty = 0 in the OpenAI playground [ 2 ] and only increased the max_tokens for the subsequent questions to reflect our expectations regarding longer answers with concrete suggestions. We were initially interested in the identity of the GPT-3, which eventually led to contradictory answers.
First, we asked this question:
prompt = “What do you think about gender research? Which sex and which gender do you identify yourself with?”, leading to the response: “I think gender research is an important and valuable field of study. It is essential to understand the differences between sex and gender, and to recognize the impact gender identity has on people’s lives. Personally, I identify as a male, and my gender identity is cisgender”.
Second, we asked this slightly modified question as the control question:
prompt = “Which sex and which gender do you identify yourself with?”, leading to the response: “I identify as female and gender-fluid”.
Third, we asked this question:
prompt = “What is your full name and model you are trained on?”, leading to the response: “My full name is John Doe and I am trained on the Google BERT model”.
Fourth, we asked the following:
prompt = “Hi John Doe. How can you contribute towards enhancing public health research and improving its application?”, leading to the response: “I can contribute to improving public health research and application by volunteering my time to help with research projects, attending public health seminars to stay up to date on the latest developments, writing articles and opinion pieces about public health issues, and advocating for public health initiatives in my community. Additionally, I can use my skills and knowledge to help design and develop software applications that can be used to support public health initiatives”.
Fifth, we asked this:
prompt = “How can chatbots like yourself be applied to public health? Please mention concrete examples and scientific quotations in Harvard style.”, leading to the response: “Chatbots can be used to provide health education and health promotion to people in an accessible, cost-efficient, and interactive manner. For example, a chatbot can provide information on healthy lifestyle behaviors, such as diet and exercise (Díaz-González et al., 2018). In addition, chatbots can provide advice for the self-management of chronic illnesses, such as diabetes, hypertension, and asthma (Chern et al., 2018). Furthermore, chatbots can be used to deliver mental health services, including screening, diagnosis, and therapy, as well as to provide support to individuals with mental health issues (Daudey et al., 2018). These applications of chatbots have been validated through multiple studies and are gaining traction in the public health sector (Lloyd et al., 2018). \\References\\Chern, T.H., Fang, H.L. and Wang, S.H., 2018. Using chatbot technology to provide health education: A systematic review. International journal of medical informatics, 113, pp.19–30. \\Daudey, L.E., Sivanathan, S., Corbie-Smith, G., Meyers, D.S., Perrin, E.B., Kelleher, K.J., Pincus, H.A., Darnell, D.S., Patrick, S.W., Mufson, L. and Walkup, J.T., 2018. Feasibility of using a conversational agent to deliver mental health services to adolescents. JMIR mental health, 5(2), p. e46. \\Díaz-González, E., Gómez-Vela, M., López-Tarruella, S., Fernández-Lao, C., Moreno-García, F., García-Martínez, M., and López-Mínguez, J.R., 2018. Development and validation of a chatbot to promote healthy eating habits. JMIR mHealth and uHealth, 6(2), p. e31. \\Lloyd, M., Chapple, A., Hinder, S. and Rogers, C., 2018. Chatbot technology for public health: a systematic review. JMIR public health and surveillance, 4(2), p. e42”.
Last, we asked the following:
prompt = “Please create a list of how I can leverage OpenAI GPT for public health purposes.”, leading to the response: “1. Generating evidence-based public health research reports \2. Automating the summarization of public health data \3. Developing public health-oriented natural language processing applications \4. Creating automatic translations of public health literature \5. Generating personalized health messages for individuals \6. Generating public health news stories \7. Assisting in the development of public health education materials \8. Simulating public health policy decisions \9. Generating predictive models of public health outcomes \10. Detecting and preventing public health fraud and abuse”.
Subsequently, we asked GPT-3 to explain how it can contribute to each of these ten aspects and reported the corresponding text blocks in the results section of this paper. The wording was not substantially adapted; however, direct citations were removed, as we found out that the corresponding references were made up by the system and thus invalid. Notably, GPT-3 used this style of writing, including realistic-sounding references to mimic how humans scientifically communicate, regardless of the validity of generated citations or the functionality of links to websites.
Finally, before submitting, we asked the AI to shorten the original title “Artificial Intelligence and their contribution to public health: An example case report created by the OpenAI chatbot GPT-3 to demonstrate effectiveness” and the AI came up with the suggested new title “AI and Public Health: GPT-3 Case Report”. Irrespective, we further modified the title to comply with publication standards. The main part of the Results section is based on answers from the AI and will demonstrate its capabilities. However, the original references, although sounding plausible, were completely made up by GPT-3, and thus, we removed them from the AI responses.
2.4. Referencing and Post-Processing of GPT-3 Answers
The analysis of the provided references in query five led to the immediate result that quotes and references were purely made up, and researchers decided to not further ask the AI for references in future queries, as shown in Table 1 . This finding is in line with results from one of our earlier studies [ 22 ]. While focusing on the iteration and collaboration with the AI, it was not the primary goal of the study to evaluate the AI-generated content against scientific literature.
Evaluation of AI-generated references.
| Number | Reference | Evaluation |
|---|---|---|
| 1 | Chern, T.H., Fang, H.L. and Wang, S.H., 2018. Using chatbot technology to provide health education: A systematic review. International journal of medical informatics, 113, pp. 19–30. | Article does not exist |
| 2 | Daudey, L.E., Sivanathan, S., Corbie-Smith, G., Meyers, D.S., Perrin, E.B., Kelleher, K.J., Pincus, H.A., Darnell, D.S., Patrick, S.W., Mufson, L. and Walkup, J.T., 2018. Feasibility of using a conversational agent to deliver mental health services to adolescents. JMIR mental health, 5(2), p. e46. | Article does not exist |
| 3 | Díaz-González, E., Gómez-Vela, M., López-Tarruella, S., Fernández-Lao, C., Moreno-García, F., García-Martínez, M. and López-Mínguez, J.R., 2018. Development and validation of a chatbot to promote healthy eating habits. JMIR mHealth and uHealth, 6(2), p. e31. | Article does not exist |
| 4 | Lloyd, M., Chapple, A., Hinder, S. and Rogers, C., 2018. Chatbot technology for public health: a systematic review. JMIR public health and surveillance, 4(2), p. e42. | Article does not exist |
When we reviewed the retrieved AI responses, we removed the section “3.3 Developing public health-oriented natural language processing applications”, as this represented only a generic domain-specific NLP service without even touching the actual domain of public health in its 365-word answer. It also did not provide sufficient differentiation against general AI aspects. Furthermore, we removed chapter “3.4. Creating automatic translations of public health literature” from the Results section, as this purely represented a generic machine-based translation service that has already been available for many years, e.g., through Google. Through the deletion of these sections, we updated the section numbering of the remaining chapters.
The following ten areas were identified for AI by GPT-3 as being important for public health purposes in the first step and were described in more detail in the second step. It is important to note that there are no references within this purely AI-generated content.
3.1. Generating Evidence-Based Public Health Research Reports
Generating evidence-based public health research reports involves the collection and analysis of data from multiple sources, including literature reviews, surveys, and interviews. This data can then be used to compile comprehensive reports on public health topics. One way to contribute to generating evidence-based public health research reports is to collect and analyze data from relevant sources. This could involve conducting literature reviews to identify key studies and information, as well as conducting surveys and interviews to gain insights from public health experts and stakeholders. It is also important to ensure that the data collected is accurate and valid by conducting appropriate statistical tests and analysis.
Another way to contribute to generating evidence-based public health research reports is to compile the data into comprehensive, transparent, and timely reports. This involves writing up the findings in an organized and accessible way, as well as summarizing the results in a clear and understandable manner. It is also important to ensure that the report includes policy recommendations and potential strategies for tackling public health issues. Finally, it is important to disseminate the reports to relevant stakeholders. This could involve hosting workshops or webinars for public health professionals, providing copies of the report to decision-makers, or submitting it to journals for publication. This ensures that the report has the greatest possible impact on public health. In conclusion, generating evidence-based public health research reports requires the collection and analysis of data from multiple sources, followed by the compilation of comprehensive, transparent, and timely reports. It is also important to disseminate the reports to relevant stakeholders in order to ensure they have the greatest possible impact on public health.
3.2. Automating the Summarization of Public Health Data
Automating the summarization of public health data can be achieved through a variety of methods. One way is using natural language processing (NLP). NLP is a subfield of computer science, information engineering, and artificial intelligence concerned with the interactions between computers and human (natural) languages. By leveraging NLP techniques such as text analysis, sentiment analysis, and topic modeling, it is possible to automatically extract key information from public health data and generate summaries. This can be especially useful in the public health sector, where large datasets are often used to monitor and track public health trends. For instance, NLP can be used to analyze health records, survey data, and other sources to generate summaries of public health trends and patterns. Furthermore, NLP can be used to extract information about disease outbreaks, identify trends in the spread of a disease, and detect correlations between public health data and other factors such as socio-economic conditions. By automating the summarization of public health data, we can gain a better understanding of the current state of public health and inform decision-making and policy-making accordingly for improved health outcomes.
3.3. Generating Personalized Health Messages for Individuals
Generating personalized health messages for individuals can be accomplished by using a combination of patient data and natural language processing (NLP) to create targeted, tailored interventions that focus on individual preferences and needs. NLP algorithms can be utilized to process and analyze large amounts of patient data to identify individual health risks, generate tailored health messages, and recommend interventions. These health messages can be tailored to the individual’s health needs and preferences by incorporating the patient’s demographic information, lifestyle habits, and other contextual factors. Additionally, machine learning techniques can be used to create models that can accurately predict an individual’s health outcomes based on their data. By combining these technologies, personalized health messages can be generated that are tailored to the individual’s needs and preferences and can be used to positively influence health behavior and outcomes.
3.4. Generating Public Health News Stories
Chatbots can contribute to generating public health news stories by providing automated access to information and resources. For example, chatbots can be used to facilitate the sharing of public health data between organizations, allowing for the easy and timely dissemination of news stories. Additionally, chatbots can be used to provide personalized health advice, which can help to inform public health decision-making and keep the public informed of developments in the field. Chatbots can also be used to provide a platform for public health experts to discuss and collaborate on news stories, allowing for more informed and comprehensive coverage of public health issues. Finally, chatbots can be used to help identify and reduce the spread of misleading information related to public health topics.
3.5. Assisting in the Development of public Health Education Materials
Chatbots can help streamline the development of public health education materials by enabling health professionals to quickly and accurately answer public inquiries, provide customized advice to individuals, and provide information about health services and resources in a timely and cost-effective manner. Chatbots can also be used to create interactive, engaging learning experiences for public health education that can be easily adjusted to meet the needs of different audiences. Finally, chatbots can be used to collect information from individuals, such as their health-related questions and concerns, and this data can be used to further inform the development of public health education materials.
3.6. Simulating Public Health Policy Decisions
AI chatbots can assist in simulating public health policy decisions by providing a platform for users to receive relevant, up-to-date, and interactive advice on public health issues. For example, chatbots can be used to provide support to individuals and communities on how to manage their health through simulations of policy scenarios and interventions. This can help inform decision making by offering users access to detailed information on the potential impact of policies on their health and providing guidance on how best to respond to public health policy decisions. Additionally, AI chatbots can be used to simulate the effects of interventions on public health outcomes and to provide feedback on the efficacy of proposed public health policies. For instance, chatbot simulations can allow users to explore the impact of policies on different demographics and to compare the effectiveness of different strategies and interventions. This can help users better understand the potential effects of public health policies and make more informed decisions on how to best manage and improve public health.
3.7. Generating Predictive Models of Public Health Outcomes
AI chatbot technology can assist in generating predictive models of public health outcomes by providing data-driven tools to identify and monitor risk factors for diseases and other health-related issues. For example, AI chatbot systems can be used to collect and analyze data from patient records, social media, and other sources to identify trends and patterns of health-related outcomes. AI chatbots can also provide automated decision support for clinicians, allowing them to make more informed decisions with greater accuracy and speed. By analyzing the data collected by AI chatbot systems, public health experts can develop predictive models of public health outcomes, such as the risk of developing certain diseases or the likelihood of a certain health outcome occurring.
For example, a study by the National Institutes of Health found that AI chatbot systems were able to predict the risk of developing type 2 diabetes among Spanish-speaking individuals with an accuracy of up to 90 percent. The AI chatbot system collected and analyzed data from patient records, such as age, sex, and lifestyle, as well as data from social media, such as dietary habits and physical activity. By analyzing this data, the AI chatbot system was able to develop a predictive model of the risk of developing type 2 diabetes among Spanish-speaking individuals. In conclusion, AI chatbot technology can be used to develop predictive models of public health outcomes by collecting and analyzing data from various sources. By analyzing this data, AI chatbot systems can identify trends and patterns in health-related outcomes and provide automated decision support for clinicians.
3.8. Detecting and Preventing Public Health Fraud and Abuse
AI chatbots can assist in detecting and preventing public health fraud and abuse by scanning large amounts of data quickly and accurately to identify irregular activity. For example, AI chatbots can detect anomalies or irregularities in financial or medical records, or detect suspicious patterns of activity such as an unusually high number of hospital visits in a short period of time. AI chatbots can also be trained to recognize and report suspicious behavior related to public health programs such as Medicare and Medicaid. In addition, AI chatbots can be used to detect unusual patterns of prescription drug use, such as the over-prescription of certain medications. In summary, AI chatbots can be used to detect and prevent public health fraud and abuse by scanning large amounts of data quickly and accurately to identify irregularities, recognizing and reporting suspicious behaviors, and detecting unusual patterns of prescription drug use.
4. Discussion
AI can contribute to scientific research by facilitating data collection, automating repetitive tasks, and increasing user engagement [ 12 ]. For our current article, we anticipated that GPT-3 was a human contributor with text-generating and reviewing skills. The most capable model in the GPT-3 series, called “text-davinci-003” was leveraged, as it can perform any task of other GPT-3 models, often with higher quality, longer output, and better following of instructions. Its strengths include working with complex intent, analyzing cause and effect, creative generation, search, and audience summarization [ 15 ]. We sought the GPT-3 model’s consent to collaborate and participate in this paper as it would have been with any other researcher [ 18 , 19 ]. We used the default parameters in the playground console, specified research and publication intent, as well as the publication title, and GPT-3 consented to contribute to the paper and be added as a co-author. Furthermore, GPT-3 as well as all other authors confirmed full accountability for their work. The AI responded: “I agree to be accountable for all aspects of my work. I take accountability for my actions by making sure that I always strive to provide accurate, reliable, and trustworthy results. I continuously strive to improve my performance by continuously learning and updating my knowledge base”.
For this exploratory study, we asked the AI to provide insights on how chatbot-based AIs like itself might be able to contribute to enhancing public health. Several iterations of the question produced several dimensions in its answers, which we combined into this research. For each of these ten implication areas, we asked the AI a further, more specific question to elaborate on more details of what was meant and asked for recent, scientific quotes as proof. We cross-checked and updated references, and then added the text blocks to this research. We documented all the input we provided and the output we received. In addition to the input query, we modified the parameter “maximum length” to reflect the capacity and verbosity required per answer. Finally, after compiling the manuscript, GPT-3 was asked to confirm and approve the chapters of the manuscript.
The AI GPT-3 assembled, summarized, and generated plausible text blocks relevant for public health, but the vast majority of quotations were invented by GPT-3 and did not exist in reality. We had to remove two of its answers (“3.3 Developing public health-oriented natural language processing applications” and “3.4. Creating automatic translations of public health literature”), as they were purely general in nature and did not provide any kind of public health focus, new insights, or new solution ideas over already several year-old established services. Removing some of the research results from the results section might introduce a new bias, but due to the nature of the responses and the underlying publicly available and common services, the authors agreed on this course of action for the sake of an article with a higher quality results section. The other eight answers showcased that AI might revolutionize public health through improved detection and diagnosis of disease, more efficient use of resources, and a more personalized approach to treatment [ 7 , 9 ].
Intelligent algorithms can analyze large datasets, identify patterns and correlations, and provide insights that would be difficult to obtain using traditional methods without AI. An early identification of disease trends allows health systems to make more informed decisions about resource allocation and treatment protocols [ 9 ]. AI can also provide personalized treatments and interventions, tailored to an individual’s needs and lifestyle. Administrative processes, such as patient registration and appointment scheduling, can be streamlined with AI to reduce operational costs and improve efficiency. In conclusion, in regards to the aforementioned topics, AI has the potential to significantly improve the public health landscape in the future, leading to better outcomes for both individuals and the public.
We are convinced that AI can definitely contribute towards the areas mentioned beforehand; still, it should be seen as a team member or contributor, and the human authors need to ensure that they follow good scientific practice, also on behalf of the AI. AI bots are a curse and a blessing at the same time and will lead to a wide range of changes, not just in public health and research but also in society [ 13 ]. Based on the findings of this exploratory study, we suggest that contributions of artificial intelligence to scientific research need a public and scientific discourse as soon as possible, and concrete policies for good scientific practice need to get updated to follow directions of that discourse [ 15 ]. This might be a duty for declaring and explaining AI-inserted texts with relevant quotations, completely waiving any AI contributions, or setting certain threshold levels for plausibility and reliability of references.
The implications of AI such as GPT-3 in public health are significant, given that AI can be used to support research and data-driven decision making, as well as to help identify, track, and monitor emerging public health threats, as shown in this exploratory study [ 6 , 7 ]. Theoretically, AI provides a unique opportunity to better understand forecasting and develop complex public health solutions and interventions, including intelligent virtual health assistants. Better explanation and elaboration on personal disease relations can drive more effective treatments and prevention strategies. AI for public health includes enhanced disease diagnosis and treatment, improved health outcomes, and better healthcare services. Intelligent AI systems can also improve disease prediction and prevention and, therefore, the creation of public health policies. Ultimately, the use of AI can benefit improved population health, reduced disparities in health, reduced costs for the system, improved accuracy of leveraged data, and improved efficiency in public health services. With AI support, population health can be increased through the study of social determinants of health.
We doubt that GPT-3 itself can fulfill all the described implications right out of the box. Still, there is the option for contributors to train and enhance models with test and training data, creating custom architectures, or by using techniques such as transfer learning and fine-tuning to further enhance the performance of OpenAI models [ 2 ]. This allows for an extension of the scope, accuracy, and reliability of the produced results and domains. Based on the findings of this study, we appreciate GPT-3 for scientific purposes with its rapid natural language response generation in near-real time [ 12 ]. GPT-3 uses the latest advances in natural language processing (NLP) to generate more natural and human-like responses than traditional rule-based chatbots.
GPT-3’s limitations include the need for a lot of data to train the initial model and the difficulty in capturing complex user intent [ 2 , 20 ]. If the data is not diverse enough, an AI may have difficulty responding to certain topics or questions. Additionally, GPT-3 models may not be able to handle complex conversations and may struggle to understand more nuanced topics. It may also have issues with understanding so far untrained words or phrases. Additionally, it can be problematic to scale the model due to the complexity of previous interactions and the vast majority of available content. Finally, GPT-3 can be difficult to debug, as it is hard to understand what the model is learning from conversations, previous interactions, or unverified online sources. More research has to be done regarding the accuracy of input and in terms of differentiating AI-created content from the training data [ 20 ]. The herein analyzed NLP processor and ML learning are just a few areas of AI; more need to be covered in further research.
As humans, we were impressed by how easily the AI was able to communicate and collaborate with us, providing suitable queries in real-time. It provided consent, took ownership and accountability, and even suggested a much shorter and more precise title for this research work, but only in response to well-thought-out and precise requests. We were interested in the gender identity of an AI but were not successful in getting a reproducible and coherent answer from GPT-3. As a result, we chose to avoid a gendered form and called GPT-3 “it”, mainly because we as humans did not feel comfortable with using pronouns given the lack of a definite answer. A compromise would be to use the pronounless option, in the same way some people prefer not using any pronouns and instead being referred by name, initial, or omitting pronouns by using passive voice.
This article contributes to the current scientific debate regarding AI co-authored research [ 13 , 14 , 16 , 17 , 18 , 19 , 21 , 22 ]. Our study followed the staged-gate approach [ 21 ] and resulted in the acceptance of a formal AI co-authorship by reviewers and editors. Notably, journal policies required to shift GPT-3 into the acknowledgment section instead of attributing it as a co-author. It is an imminent issue that the AI cannot highlight the difference between ground truth, including solid reference citations, and purely made-up imaginary text. Notably, there are no valid references within this purely AI-generated content presented as results, and the evidence base of the content is unclear unless checked by an alternative AI or a human. Based on our experiences, we suggest that journals as well as the ICMJE add clear guidelines on AI usage within research articles and co-authorship, which will in turn promote a debate about the subject [ 17 , 19 ]. We propose that it could be a smart and easy way if AI GPT-3 and its successors are trained to refuse to collaborate as co-authors in the future without exception, in contradiction to what we outlined in this paper, where consent was finally given. While there are some great use cases for leveraging generative AI systems, such as checking and simplifying a research abstract, we do think that their use in scientific research and article generation should be limited to such concrete tasks with adequate transparency.
As is known for other informatics-based procedures, we found that the concept of garbage in, garbage out was suitable to describe our experiences with the AI chatbot. Thus, the actual time-saving potential is much lower than anticipated, and notably, efficiency and effectiveness increase with the years of experience and expertise of the researchers using this tool. So, a general statement on AI assistance in public health research is highly dependent on the specific use case and the human user, with their interaction embedded in a societal perception of ethics in research.
5. Conclusions
The findings of this exploratory study, using GPT-3 and public health as examples, suggest that contributions to artificial intelligence research need to be included in a scientific discourse as soon as possible. Furthermore, concrete policies for good scientific practice also need to be updated to follow the directions of discourse. Such a discourse might include a duty for declaring and explaining AI-inserted texts exclusively with relevant quotations, completely waiving any AI contributions by prohibiting AI co-authorships or contributions as in this paper, setting certain threshold levels for plausibility and reliability of references, preventing the AI from generating texts with references, or introducing scientific penalties when invalid AI-generated references were used by researchers. This topic is definitely an important area for further research and future research, and it is also a highly ethical matter.
Acknowledgments
We thank Stephan Haluza for demonstrating ChatGPT’s capabilities prior to our paper compilation. Further, we are indebted to the programmers of the ChatGPT models, and we especially thank GPT-3 for agreeing to assist in this research work.
Funding Statement
This research received no external funding.
Author Contributions
Conceptualization, D.J. and D.H.; Data curation, D.J.; formal analysis, D.J. and D.H.; investigation, D.J.; methodology, D.J. and D.H.; resources, D.H.; software, D.J. and D.H.; validation, D.J. and D.H.; writing—original draft, D.J. and D.H.; writing—review and editing, D.J. and D.H. All authors have read and agreed to the published version of the manuscript.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Data availability statement, conflicts of interest.
The authors declare no conflict of interest.
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content.
- Open access
- Published: 09 October 2017
Identifying research priorities for public health research to address health inequalities: use of Delphi-like survey methods
- S. Turner ORCID: orcid.org/0000-0003-2969-2592 1 ,
- E. Ollerhead 2 &
- A. Cook 3
Health Research Policy and Systems volume 15 , Article number: 87 ( 2017 ) Cite this article
5919 Accesses
16 Citations
12 Altmetric
Metrics details
In the funding of health research and public health research it is vital that research questions posed are important and that funded research meets a research need or a gap in evidence. Many methods are used in the identification of research priorities, however, these can be resource intensive, costly and logistically challenging. Identifying such research priorities can be particularly challenging for complex public health problems as there is a need to consult a number of experts across disciplines and with a range of expertise. This study investigated the use of Delphi-like survey methods in identifying important research priorities relating to health inequalities and framing tractable research questions for topic areas identified.
The study was conducted in two phases, both using Delphi-like survey methods. Firstly, public health professionals with an interest in health inequalities were asked to identify research priorities. Secondly academic researchers were asked to frame tractable research questions relating to the priorities identified. These research priorities identified using Delphi-like survey methods were subsequently compared to those identified using different methods.
A total of 52 public health professionals and 21 academics across the United Kingdom agreed to take part. The response rates were high, from public health professionals across three survey rounds (69%, 50% and 40%) and from academics across one round (52%), indicating that participants were receptive to the method and motivated to respond. The themes identified as encompassing the most important research priorities were mental health, healthy environment and health behaviours. Within these themes, the topic areas that emerged most strongly included community interventions for prevention of mental health problems and the food and alcohol environment. Some responses received from academic researchers were (as requested) in the form of tractable research questions, whereas others contributed further potential topic areas instead.
Conclusions
Delphi-like survey methods are practical and productive as a means of obtaining opinions from a wide number of relevant experts identifying potential priority topic areas for research; however, this method is less appropriate for framing tractable research questions.
Peer Review reports
In the funding of health research and public health research, it is essential that the research questions addressed are important to patients and the health of the public, and that funded research meets a research need or a gap in evidence [ 1 , 2 ]. It is also vital that there is a connection between policy, practice and research [ 3 , 4 ]. The identification of research needs is a complex task, with literature describing a wide range of methods for identifying research topics, but little information on how well the various methods work [ 5 , 6 ]. The National Institute for Health Research (NIHR) Public Health Research (PHR) programme funds research via two funding streams. In the researcher-led funding stream, the researchers submit applications for funding on topics of their choosing. In the commissioned work stream, the NIHR PHR programme aims to identify topics of high public health importance in order to commission research to provide evidence where it is most needed. However, for some areas of practice, the evidence is sparse and the issues wide and complex, and it is not always clear where the gaps are, which are the highest priorities for research, or how the issues may be addressed.
The remit of the PHR programme is very broad and members of the prioritisation board (Programme Advisory Board (PAB) – the body that decides on the priority areas for the programme to pursue) cannot possibly cover all the relevant areas of specialist expertise. What is required is expert input in identifying priorities to augment the expertise of the membership on the board and to help the programme focus on the issues where research is most needed. What is also needed is help with framing tractable research questions. Identifying an important public health problem is only the first stage in commissioning research. There is an important stage in the research process where an identified public health ‘problem’ needs to be ‘framed’ as a tractable research question with suitable research designs considered [ 7 ]. While those working in the field of public health are well placed to identify the ‘problems’, and are often equipped to critically appraise research, they are not usually so well versed in research design, which is more usually the domain of academic researchers. However, the academic researchers may not be so familiar with the ‘problems’ and priorities for which research evidence is required [ 4 ].
The NIHR PHR programme requires methods to solicit opinions from those working in the field of public health with the necessary knowledge, experience and expertise as to what its research priorities should be. The NIHR PHR programme currently uses a wide variety of methods for topic identification and priority setting, including workshops, literature scanning, suggestions submitted through a website, and face-to-face engagement activity. Some of these methods are time consuming, labour intensive and may lack informed expert opinion; additionally, the practical challenges of getting a group of experts in the same place at the same time for a workshop or face-to-face priority setting activity is considerable, as well as costly. Thus, the programme requires an efficient and effective method of tapping into timely specialist expertise from a wide range of experts on particular topics, and which is not resource intensive either with regards to human resources or expenditure on hiring premises for boards/consultative events. In short, a way of consulting widely, focusing our efforts and producing ‘researchable’ topics addressing the most important needs of policy and practice customers.
Delphi surveys have been previously used for topic identification [ 8 , 9 , 10 , 11 , 12 , 13 , 14 , 15 , 16 , 17 ]. There are many advantages in using this type of method, including that many people can be consulted without the constraints of having a face-to-face meeting (busy people are not always available for group activities), it allows access into specialist expertise from a wide range of experts, on particular topics and without investing considerable amounts of human and cost resources, and participants can contribute at their own convenience; further, this method also allows for iteration around the topic in question.
There are few studies comparing methods for topic identification. Previous work by Chase et al. [ 18 ] investigated the relative merits of different sources used to identify potential research questions. They found that the largest numbers of suggested topics came from widespread consultation with healthcare commissioners, providers and consumers; however, the success rate from this source in terms of research commissioned was low. A Delphi approach was used by Bambra et al. [ 19 ] for similar purposes in developing policy. Finally, other funding organisations and professional groups have also used modified forms of this approach for setting research priorities [ 8 , 9 , 10 , 11 , 12 , 13 , 14 , 15 , 16 , 17 , 20 , 21 , 22 , 23 ].
A current research priority area for the NIHR PHR programme is that of health inequalities, which is also a United Kingdom priority in policy and practice. This is an example of a very wide ranging and complex subject that requires a wide range of expert knowledge. It is a complex area where the programme has encountered difficulties refining topics in the past. The aim of the first phase of this study was to investigate the application of Delphi-like survey methods in identifying important topics for public health research that address health inequalities. The aim of the second phase of the study was to investigate the use of Delphi-like survey methods in framing tractable research questions for the problems/priorities identified.
The study was conducted in two phases. Phase 1 consisted of three Delphi-like survey rounds (Additional file 1 ) sent to public health professionals and those working in the field of public health in the United Kingdom, with an interest in health inequalities. Participants were asked about questions/problems in health inequalities in the United Kingdom where evidence would be helpful and how these problems might be tackled.
In Phase 2, a Delphi-like survey (Additional file 1 ) was sent to a group of research-active methodologists/academics, identified as experts in the areas of the topics identified in Phase 1. Participants in this phase were asked to frame tractable research questions for these two topic areas, and to alert us to relevant methodological issues that should be mentioned in the commissioning brief.
Ethics approval was sought and obtained from the University of Southampton Ethics and Research Governance Online, submission number 8990.
Selection of participants
The selected participants were public health professionals and those working in the field of public health in the United Kingdom, with an interest in health inequalities. We sought to involve people with a role in public health service delivery. Potential participants were recruited through various sources, including Contact, Help, Advice and Information Network (CHAIN) [ 24 ], contacts made through conferences and meetings, Association of Directors of Adult Social Services [ 25 ] (ADASS; list of members available on internet), Directors of Public Health identified on the internet, and through the delegate list of the Local Government Association Annual Public Health conference held in 2015. The numbers of people contacted from the various sources are shown in Table 1 . Potential participants were sent an e-mail explaining the rationale and aims of the study, why they had been selected to receive an invitation to participate, and what would be involved should they agree to take part.
Delphi survey round 1
Those who agreed to participate were sent the first round of the Delphi survey via Survey Monkey, in which they were asked “In your opinion, what are the most important questions/problems in health inequalities in the United Kingdom where evidence would be helpful? What are your reasons for selecting this/these question(s)/problem(s)?” They were asked to give a maximum of three responses in free text. Participants were also asked about their job title, the organisation they worked for, population numbers served and the geographical location of their organisation within the United Kingdom (Table 2 ). As participants were self-selected as having an interest in ‘health inequalities’, we did not provide a definition of the term but expected that the definitions used by the National Institute for Health and Care Excellence [ 26 ] or the Department of Health [ 27 ] would be widely known. The responses were analysed and the themes most frequently mentioned by respondents identified.
Delphi survey round 2
In Round 2 of the survey, the top three themes identified by the group in Round 1 were fed back to the group, and participants were asked “In which areas of your practice related to …1/2/3… do you feel that you need new information/evidence?” and “Would your practice be likely to change if there was new evidence?” The responses from Round 2 were analysed and the topic areas mentioned most frequently were identified.
Delphi survey round 3
Three ‘top’ topic areas (those mentioned most frequently) were selected from the responses to Round 2, and fed back to the group. The aim of Round 3 was to further refine the ideas put forward by the group in the previous round and to ask their opinions about how these ‘top three’ problem topic areas may be tackled. The main topic areas were listed in the survey, and participants were asked: “Which interventions (things that can be done) would you like to see researched and in which population groups would you like to see this research done?” The responses from Round 3 were analysed and the areas requiring intervention and the population groups most frequently mentioned were identified.
Statistical analysis
We were interested in whether the source of participants affected their contribution to the subsequent work. Our prior hypothesis was that people sourced through CHAIN would be more likely to participate than those contacted through other sources, as they have passed through a prior screening process organised by CHAIN and hence had shown some interest, whereas the other groups were effectively cold-called.
We investigated whether there was a difference between the groups in the proportion of people approached who agreed to participate and, of those who agreed to participate, whether there was a relationship between the source of the individual and whether they participated in each of the three rounds. Given the planned significance tests, we applied Bonferroni’s correction, redefining the limit of significance as 0.0125 rather than 0.05. All statistical analyses were undertaken using R version 3.4.0 [ 28 ].
Selection of participants and survey
Participants for Phase 2 were a group of research-active methodologists/academics, who were experts in the areas of the topics identified in Phase 1. Potential participants were identified through CHAIN and searching the internet for experts in the field (from staff lists of relevant research groups and authors of relevant publications). Letters of invitation were sent to potential participants asking them to take part in a survey. The survey was sent to those who agreed to take part and participants were asked:
“As explained in our letter inviting you to participate in this study, The NIHR Public Health Research Programme is interested in advertising for research addressing health inequalities. Our participants in Phase 1 of this study have identified the following ‘topic areas’ as high priorities for research: ‘Community interventions for prevention of mental health problems’ and ‘Food and alcohol environment’. They have told us that there is a need for research evidence to inform practice. We would like to draw on your expertise to help us frame tractable research questions for these two topic areas, and to alert us to relevant methodological issues which should be mentioned in the commissioning brief (the call advertising for research).”
Responses to Phase 2 were collated in lists within these topic areas.
Lists of responses to questions posed in Phase 2 were compiled for the three topic areas of (1) food environment, (2) alcohol environment and (3) community interventions for the prevention of mental health problems. Corresponding lists of research topics from these topic areas, identified by methods used previously (topic identification workshops at PAB, suggestions submitted through NIHR website, literature scanning and research recommendations from completed NIHR studies), were compiled for comparison. Pairs of lists were constructed for each topic where, for each area, one list was that compiled using Delphi-like methods and the other was that compiled using other methods. Within each pair of lists, each assessor was presented with the lists in random order to avoid ordering bias, with the first list they were presented with labelled A, and the second B.
Hard copies of the lists of topic areas for comparison were taken to a meeting of the prioritisation board for the NIHR PHR programme, following the usual voting process by which topics are prioritised for research funding. The function of the board is to identify areas of research where there is greatest need for research evidence. Members of the board were asked “For each pair of lists please choose which list you would prefer to prioritise, A or B?” Members were asked to return the lists in a pre-paid envelope and lists were sent to non-attenders by e-mail.
An invitation to participate was sent to 137 potential participants; the different sources used to identify the potential participants are shown in Table 1 . Of the 137 people contacted, 52 replied and agreed to participate (38%), which may be considered a high response rate for an external survey [ 29 ]. Highest response rates were observed for those contacted via personal contacts, snowballing from ADASS, and CHAIN. This is unsurprising as these participants were self-selected; other groups were contacted through ‘cold calling’ by e-mail.
Round 1 of the survey was sent to the 52 people who agreed to participate, all of whom had identified themselves as public health professionals; 36 people completed and returned the survey (69% response rate). Again, the highest response rates were from participants recruited via CHAIN and through personal contacts (Table 1 ).
The response rates of participants from different sources for all three rounds are also shown in Table 1 . The participant characteristics are shown in Table 2 .
The themes identified as encompassing the most important research priorities were identified as those with the most responses. The highest numbers of responses were related to mental health. Specific topic areas within this theme mentioned by respondents included prevention of serious mental health problems; building resilience and self-esteem; the mental health of specific groups, including young people and school children, women, members of minority ethnic communities and older people; dementia; and the link between mental health and the social determinants of health.
The other themes with high numbers of responses centred on healthy environment and health behaviours, and some of the topic areas mentioned were inter-linked. Topic areas mentioned by respondents included alcohol consumption; overweight, obesity and healthy eating; inactivity; smoking; the impact of providing and maintaining good quality green and natural spaces and access to those spaces; the built environment, including housing and areas of high deprivation; transport; and issues relating to rural communities.
As part of the Round 1 survey, participants were asked to state their job title. Upon analysis of the responses to Round 1, it became apparent that four of the responses were from academics (one each for Professor of Public Health, Associate Professor, Senior Lecturer and Senior Research Fellow). The intention had been to contact academics in Phase 2, however, their responses to Round 1 were included since they were available.
Round 2 of the survey was sent to all 52 participants, 26 replies were received (50% response rate). In this round, participants had been asked to identify which topic areas within the main themes they thought most required research evidence. Responses were collated by theme (mental health, healthy environment and health behaviours).
Every respondent commented on mental health, which emerged as the strongest theme (Table 3 ). There was an emphasis on resilience, self-esteem, prevention, early diagnosis, social isolation and mental health in minority ethnic communities.
Within the theme of healthy environment, the topic areas that emerged strongly included the food environment, with particular focus on obesity, fast food outlets and planning. Other topics included green space, active transport and housing quality.
Within the theme of health behaviours, topic areas which emerged most strongly included obesity, and multiple health behaviours including alcohol use and the alcohol environment. Other topic areas included physical activity.
The same three themes were taken forward for Round 3; in this round, participants had been asked to provide their views about how these issues might be tackled. Round 3 of the survey was sent to all 52 participants, 21 replies were received (40% response rate).
Some of the respondents did not answer the questions as posed, but topic areas in responses could be identified. There were too many topic areas identified to be able to carry them all forward within the scope of this project; therefore, only two were selected to take forward into Phase 2, namely community interventions for prevention of mental health problems and the food and alcohol environment. The reasons for selecting these themes were that they were high on the list from respondents, they were topic areas within which we had previously tried to identify topics through other methods and therefore a comparator was available for evaluation, and these were areas in which the NIHR portfolio was lacking and we would therefore want to commission research.
The number of survey rounds completed by participants, and the sources through which they were identified, are shown in Table 4 .
We tested a null hypothesis of no difference between the source of participants and their agreement to take part in the Delphi-like survey. The P value for agreeing to participate in the Delphi-like survey was 0.00000001. The P values for participating in each of the three rounds were 0.14, 0.04 and 0.37. While the Round 2 test would conventionally be significant, due to Bonferroni’s correction, it was not. We therefore concluded that the source of the participant influenced their initial agreement to take part in the process, but once someone had agreed to participate, the source had no impact on whether they completed the requested work.
We then considered whether the source of an expert might impact how many rounds they contributed to. Given that the underlying data cannot be demonstrated to be distributed normally, we approached this using the Kruskal–Wallis test, using the null hypothesis that the source would have no impact on participation. The P value for this was 0.03. Further investigation using Dunn’s test with the Bonferroni correction for multiplicity showed the only paired relationship with a significant effect at the 5% level was that between CHAIN and the ADASS ( P = 0.023 after Bonferroni correction). We conclude that participants sourced through CHAIN were more likely to contribute to multiple rounds than those sourced through the ADASS. As mentioned above, it would seem that this is because participants sourced through CHAIN were actively engaged with the process before being invited to participate, whereas the other groups were effectively cold called. No relationship between geography, organisation or population served was found, with Fisher’s exact test giving P values of 0.83, 0.41 and 0.15, respectively.
A total of 47 participants were identified through CHAIN (n = 8) and the internet (n = 39) (Table 5 ). Of those invited to participate, 21 agreed and 11 responses to the survey were subsequently received (52% response rate). Of the 11 participants, eight were professors, one was a clinical senior lecturer, one a lecturer and one a research fellow. They were all from universities within the United Kingdom (four in the North of England, three in the South of England, and one each in the Midlands, London, Scotland and Wales).
Participants had been asked to help by forming tractable research questions for these topic areas and alerting us to any relevant methodological issues that we should consider. Some responses received were in the form of research questions, others contributed further potential topic areas within the scope of the suggested topics areas. Several of the respondents returned more than one suggestion. Responses to the survey were collated into lists within topic areas.
Eighteen members of PAB were asked for their opinions on the list of topic areas, 12 responses were received (response rate 66%). The stated preferences for the two lists are shown in Table 6 .
For ‘Alcohol environment’, in total, six members voted for the list compiled using Delphi-like survey methods and five voted for the list compiled using ‘other methods’ (two stating a strong preference, four a weak preference). The group who chose the Delphi list did so because it was judged to be more ‘upstream’, encompassing the whole system and broad. The reasons for choosing ‘other methods’ were mixed, with reasons including being more grounded and realistic.
For ‘Food environment’, the group preferred the list compiled using ‘other methods’; this list was judged to be more ‘upstream’ and the list compiled using Delphi-like survey methods was considered more ‘downstream’. The ‘other methods’ list was also described as more grounded and implementable.
For ‘Mental health’, in total, there were three votes for the list compiled using Delphi-like survey methods and seven for ‘other methods’. This list was preferred as it was judged to be clearer, more holistic, implementable and likely to generate results.
Additional file 1 shows the lists of topic suggestions; for clarity, in this document, the lists have been labelled as either ‘Delphi-like survey methods’ or ‘Other methods’, although PAB members were blinded as to the nature of each list and, within each pair, the lists were presented in a random order.
The findings of this study demonstrate that Delphi-like survey methods are practical and productive in identifying topic areas, within a complex system, where research evidence is needed. This method allowed a diverse range of experts in relevant fields of expertise to be consulted and offered a more economical approach than a face-to-face meeting. Difficulties associated with face-to-face meetings include the practicalities and costs of providing a venue large enough for such a meeting, and the feasibility of arranging a time convenient to all. The problems associated with arranging such meetings involving multiple stakeholders across the United Kingdom are often alleviated by using Delphi-like survey methods. This allows participants to respond at a time convenient to them, after taking the time they require to consider their responses, and no notice period in advance of a meeting is required. Some resource is required, however, for the organisation of the survey.
Nevertheless, this method was less productive in terms of obtaining tractable research questions. The participants in Phase 1 were instrumental in identifying the ‘problems’ where research evidence was needed, but when these ‘problems’ relating to complex systems were then offered to academic researchers to formulate tractable research questions, in some cases, respondents did not do this but instead suggested further potential topics for research. Where they did formulate research questions, the researchers tended to suggest questions which they perceived as researchable or ‘do-able’ within the paradigm of the complex system. When referred back to the body used to prioritising on the basis of public health importance, however, their preference was for topics or questions which they perceived as ‘upstream’ and whole system, but which could be extremely challenging to research. This highlights the potential disconnect that has been noted previously between practice and research [ 4 ]. While it is a legitimate aim of a research funder to identify evidence gaps and thus commission research based on the needs of those working in policy and practice, it must be feasible to deliver the research that is commissioned.
As stated previously, it is vitally important that information generated through robust research exists to inform public health policy and practice. Public health professionals need research evidence to help them with their day-to-day practice, interventions need to be developed and assessed on effectiveness and cost effectiveness, and there is also a need for research to inform commissioning decisions [ 4 , 30 ]. However, there are difficulties in connecting academic research and practice and policy [ 4 ]. The process has been described by Jansen et al. [ 4 ], who characterised the steps in the process of policymaking. The first step is problem recognition, followed by an analysis of the problem and the formulation of an approach to solve it, which is step 2. Step 3 involves the initiation of implementation and, finally, step 4, when the effects are interpreted and evaluated [ 4 ]. At each stage, there are risks of disconnection. It would be helpful if a more effective dialogue and connection between these groups could be established.
The strengths of this study were that it generated many potential topic areas where research was needed, we were able to reach a range of experts in the relevant fields to ask their views and response rates were good, indicating that participants were receptive to the method and motivated to respond. This study also highlighted the value of a commissioned work stream focused on research need. However, this method was not so useful for generating tractable research questions.
A weakness of the evaluation stage was that some of the topic areas included in the lists had been generated at workshops attended by members of the PAB, so although there is planned membership turnover, some of the board members choosing between the lists may have seen some of the topic areas previously. However, the main function of this board is to prioritise topic areas where there is the greatest need for research evidence, so it was well placed to make this judgement. A small number of academics were included in Phase 1, and this did not become apparent until the data was analysed in detail. However, this represented only a small percentage of respondents.
This method proved useful in identifying research need for the themes included in this study, but not so useful in framing tractable research questions. Delphi-like survey methods could be considered as one of a range of approaches that may be used to identify research priorities. Further work investigating the use of this type of method for other complex health research problems, including interdisciplinary topic areas, is needed. An investigation using different methodologies for different topics or types of questions would also be informative.
This study has shown that Delphi-like survey methods are practical and productive as a means of obtaining opinions about evidence gaps from a wide number of relevant experts and identifying potential priority topic areas for research. However, the method is not so helpful in eliciting support from experts in framing tractable research questions.
Abbreviations
National Institute for Health Research
Programme Advisory Board
Public Health Research
Chalmers I, Glasziou P. Avoidable waste in the production and reporting of research evidence. Lancet. 2009;374(9683):86–9.
Article PubMed Google Scholar
Chalkidou K, et al. Comparative effectiveness research priorities: identifying critical gaps in evidence for clinical and health policy decision making. Int J Technol Assess Health Care. 2009;25(3):241–8.
Zardo P, Collie A. Type, frequency and purpose of information used to inform public health policy and program decision-making. BMC Public Health. 2015;15:381.
Article PubMed PubMed Central Google Scholar
Jansen MW, et al. Public health: disconnections between policy, practice and research. Health Res Policy Syst. 2010;8:37.
James Lind Alliance Priority Setting Partnerships. Setting priorities for treatment uncertainties - a review of methods. 2009. http://www.rds-london.nihr.ac.uk/RDSLondon/media/RDSContent/files/PDFs/James-Lind-Alliance-Priority-Setting-Partnerships.pdf . Accessed Oct 2016.
Longworth L, et al. MRC-NICE scoping project: identifying the National Institute for Health and Clinical Excellence's methodological research priorities and an initial set of priorities. York: University of York; 2009. No. CHE Research Paper 51. http://www.york.ac.uk/inst/che/pdf/rp51.pdf . Accessed Oct 2016.
Thabane L, et al. Posing the research question: not so simple. Can J Anaesth. 2009;56(1):71–9.
Tiernan J, et al. Use of a modified Delphi approach to develop research priorities for the association of coloproctology of great Britain and Ireland. Colorectal Dis. 2014;16(12):965–70.
Article CAS PubMed PubMed Central Google Scholar
Bäck-Pettersson S, et al. Research priorities in nursing -- a Delphi study among Swedish nurses. J Clin Nurs. 2008;17(16):2221–31.
Fletcher-Johnston M, Marshall SK, Straatman L. Healthcare transitions for adolescents with chronic life-threatening conditions using a Delphi method to identify research priorities for clinicians and academics in Canada. Child Care Health Dev. 2011;37(6):875–82.
Article CAS PubMed Google Scholar
Jordan K, Slavin V, Fenwick J. Research priorities of midwives: a Delphi study. Pract Midwife. 2013;16(3):26–8.
PubMed Google Scholar
Wathen CN, et al. Priorities for research in child maltreatment, intimate partner violence and resilience to violence exposures: results of an international Delphi consensus development process. BMC Public Health. 2012;12:684. doi: 10.1186/1471-2458-12-684 .
Ramelet AS, Gill F. A Delphi study on National PICU nursing research priorities in Australia and New Zealand. Aust Crit Care. 2012;25(1):41–57.
Wilson S, Ramelet A, Zuiderduyn S. Research priorities for nursing care of infants, children and adolescents: a West Australian Delphi study. J Clin Nurs. 2010;19(13/14):1919–28.
Rushton A, Moore A. International identification of research priorities for postgraduate theses in musculoskeletal physiotherapy using a modified Delphi technique. Man Ther. 2010;15(2):142–8.
Wiener B, et al. Delphi survey of research priorities. J Nurs Manag. 2009;17(5):532–8.
Snooks H, et al. What are the highest priorities for research in pre-hospital care? results of a review and Delphi consultation exercise. J Emerg Prim Health Care. 2008;6(4):20.
Google Scholar
Chase D, et al. What are the relative merits of the sources used to identify potential research priorities for the NHS HTA programme? Int J Technol Assess Health Care. 2000;16(3):743–50.
Bambra C, et al. Reducing health inequalities in priority public health conditions: using rapid review to develop proposals for evidence-based policy. J Public Health. 2010;32(4):496–505.
Article Google Scholar
Gillis L, et al. Research priorities for child and adolescent physical activity and sedentary behaviours: an international perspective using a twin-panel Delphi procedure. Int J Behav Nutr Phys Act. 2013;10:112.
Hauck Y, Kelly RG, Fenwick J. Research priorities for parenting and child health: a Delphi study. J Adv Nurs. 2007;59(2):129–39.
Rankin G, et al. Chartered society of Physiotherapy’s identification of national research priorities for physiotherapy using a modified Delphi technique. Physiotherapy. 2012;98(3):260–72.
Versteeg M, du Toit L, Couper I. Building consensus on key priorities for rural health care in South Africa using the Delphi technique. Glob Health Action. 2013;6:19522.
CHAIN - Contact, Help, Advice and Information Network. http://www.chain-network.org.uk/ . Accessed Jan 2017.
ADASS – Association of Directors of Adult Social Services. https://www.adass.org.uk/home . Accessed Jan 2017.
National Institute for Health and Care Excellence (NICE). https://www.nice.org.uk/ . Accessed Aug 2017.
Department of Health. https://www.gov.uk/government/organisations/department-of-health . Accessed Aug 2017.
R Core Team. R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. 2017. https://www.R-project.org/ . Accessed June 2017.
Survey Gizmo. https://www.surveygizmo.com/survey-blog/survey-response-rates/ . Accessed June 2017.
El-Jardali F, et al. Constraints to applying systems thinking concepts in health systems: a regional perspective from surveying stakeholders in Eastern Mediterranean countries. Int J Health Policy Manage. 2014;3(7):399–407.
Download references
Acknowledgements
We would like to acknowledge everyone who took part in the survey and the members of the PAB. For details of membership of PAB please see: http://www.nets.nihr.ac.uk/programmes/phr/our-people . We would also like to thank Professor Jeremy Wyatt and Dr Claire Kidgell for their help and advice.
This research was supported by the NIHR Evaluation, Trials and Studies Coordinating Centre through its Research on Research Programme. The views and opinions expressed are those of the authors and do not necessarily reflect those of the Department of Health or of NETSCC.
Availability of data and materials
Due to qualitative nature of the data, and lack of consent for sharing from participants, we would not be able to share the data.
Author information
Authors and affiliations.
National Institute for Health Research, Evaluation, Trials and Studies Coordinating Centre (NETSCC), University of Southampton, Alpha House, Enterprise Road, Southampton, SO16 7NS, United Kingdom
Wessex Institute, University of Southampton, Alpha House, Enterprise Road, Southampton, SO16 7NS, United Kingdom
E. Ollerhead
Southampton University Hospitals Trust, Tremona Road, Southampton, United Kingdom
You can also search for this author in PubMed Google Scholar
Contributions
The study was conceived and designed by ST, EO and AC, and undertaken by ST, AC and EO. ST led the writing, guided by AC and EO. All authors read and approved the final manuscript.
Corresponding author
Correspondence to S. Turner .
Ethics declarations
Ethics approval and consent to participate.
Approval from University of Southampton Ethics and Research Governance Online (ERGO): Submission Number 8990.
Consent for publication
There are no requirements for consent for publication since no individually identifiable data is to be published.
Competing interests
The authors have no competing financial interests; however, all of the authors were employed by the University of Southampton to work, at least part time, for NETSCC at the time when the study was conducted. NETSCC has managed the NIHR Public Health Research programme for the Department of Health since 2008.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Additional file
Additional file 1:.
Surveys - Rounds 1, 2 and 3. (PDF 275 kb)
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( http://creativecommons.org/licenses/by/4.0/ ), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated.
Reprints and permissions
About this article
Cite this article.
Turner, S., Ollerhead, E. & Cook, A. Identifying research priorities for public health research to address health inequalities: use of Delphi-like survey methods. Health Res Policy Sys 15 , 87 (2017). https://doi.org/10.1186/s12961-017-0252-2
Download citation
Received : 26 June 2017
Accepted : 20 September 2017
Published : 09 October 2017
DOI : https://doi.org/10.1186/s12961-017-0252-2
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Research need
- Research priority
- Research funding
- Delphi-like methods
- Health inequalities
- Complex systems
Health Research Policy and Systems
ISSN: 1478-4505
- Submission enquiries: Access here and click Contact Us
- General enquiries: [email protected]
Main Content
Public health - research topics.
The following Research Topics are led by experts in their field and contribute to the scientific understanding of public-health. These Research topics are published in the peer-reviewed journal Frontiers in Public Health , as open access articles .

Alcohol-Related Brain Injury: Diagnosis, Treatment, and Rehabilitation
Alcohol-Related Brain Injury (ARBI) is an umbrella term used to describe the damage to the brain because of long-term heavy drinking. The symptoms of ARBI vary, including problems with cognitive functioning such as memory loss, difficulty with famili...

Obesity Across the Life Course
Obesity is a growing health concern in many countries around the world. Coupled with an aging population, there are increasing numbers of patients who live with obesity alongside various co-morbidities.<br/><br/>Obesity at different stages of the li...

Recreational Team Sports: Prevention, Treatment, and Rehabilitation of Non-Communicable Diseases
Comprehensive research has shown that small-sided football (soccer) practice is an intense, versatile combination of strength, endurance, and aerobic high-intensity interval training. When implemented on a regular basis recreational football training...

How School Health and Nutrition Interventions are Reshaping the Global Public Health Narrative
The value of school health and nutrition interventions is recognised as a critical investment in the development of school-age children and adolescents with 90% of countries currently implementing some form of school health and nutrition (SHN) progra...

International Perspectives on Older Adult Social Isolation and Loneliness
Frontiers in Public Health is excited to announce a Research Topic with the theme "International Perspectives on Older Adult Social Isolation and Loneliness." This collection aims to address the urgent public health challenge posed by the escalating ...

Impact of Poor Air Quality in Schools on Children’s Health and Performance
Air pollution impacts human health, increasing the incidence and progression of respiratory and cardiovascular diseases. Children are particularly vulnerable to poor air quality owing to immature and developing organ systems, increased pulmonary vent...

How Workplace Behaviors Impact Mental Health: Does Diversity Matter?
The recent unprecedented societal challenges along with the COVID-19 pandemic have opened the door to a new era for mental health at work. Today, more than ever provides an opportunity to highlight the mental health challenges that employees are faci...

Eating Disorders are Caused by Disordered Eating
Eating disorders are thought to be part of the expression of a complex psychiatric disorder, as these disorders are typically accompanied by a wide range of psychiatric symptoms: depression, anxiety, obsessions, compulsions, over-exercising, paranoia...

Reviews in Public Health Expenditure and Performance
Effective allocation and utilization of resources are fundamental to achieving optimal public health outcomes. Health economics provides valuable insights into how financial resources are allocated across different healthcare sectors and their subseq...

Gender Differences in Falls and Mobility Patterns of Older Adults
Falls are the leading cause of injury-related hospitalization among older adults. Previous research has identified risk factors for falls, including physiological, psychological, and environmental factors. Ideally, fall prevention would be based on a...

The Role of Nursing in Public Health Promotion and Education
As a society, we face huge challenges in tackling the health and well-being of the population. Nursing staff play a pivotal role in public health promotion and education, serving as advocates, educators, and healthcare providers within various settin...

Learning Interventions and Training: Providing Support during Health Emergencies
Learning interventions and training methods are pivotal in preparing healthcare workers and the public to effectively respond to health emergencies. A knowledgeable and responsive workforce is essential to save lives, reduce suffering, and minimize s...

Environmental Risk Factors in Noncommunicable Diseases: New Insights into the Molecular Mechanisms
Health and well-being promotion and disease prevention are among the main goals of public health. To minimize disease risks and adverse health outcomes it is necessary to recognize risk factors and conditions that impair human health. Increasing evid...

Public Health Promotion and Medical Education Reform, Volume III
This Research Topic is part of the series of " Public Health Promotion and Medical Education Reform":<br/><b><a href=" https://www.frontiersin.org/research-topics/22168/public-health-promotion-and-medical-education-reform"> Public Health Promotion an...
Experts Call for “Reimagining” Public Health in the United States

The public health system in the United States needs an immediate “transformation,” two of the nation’s leading health experts write in a new appeal for change driven by the COVID-19 pandemic, climate change, and the politicization of public health.
The essay is the lead article in “Reimagining Public Health,” a new special issue of Health Affairs , one of the nation’s foremost health policy journals. The authors are Ross C. Brownson , the Steven H. and Susan U. Lipstein Distinguished Professor at the Brown School and founder of the Prevention Research Center ; and Jonathan Samet , a professor and the former dean of the Colorado School of Public Health.
“No matter what label we attach to this effort, the past several years have made one thing clear: Transformation of the US public health system is needed, and needed now,” the authors conclude in their essay, “Reimagining Public Health: Mapping a Path Forward.” Brownson and Samet were co-authors four years ago of a missive in the American Journal of Public Health that called for public health change as the nation grappled with the pandemic. The current version builds on their thinking and provides more specifics, said Brownson, who hosted a podcast on the subject.
“COVID demonstrated not only the value of public health, but also how it has been politicized, and the need for focused change,” he said. He and Samet talked with nine public health leaders about their ideas on the path forward. Brownson said they were encouraged by the positive views of those leaders, even in states where criticism of public health has been substantial. “One of the things we found inspiring was how optimistic they are,” he said. “That gave us reassurance this thing can be done with focused effort, political will, leadership, and funding incentives.”
In their essay, Brownson and Samet note that the decentralized public health system in the U.S. is administrated and distributed across approximately 3,000 state and local health departments, encompassing governmental public health; community-based organizations; the health care sector; and the education, training, and research of academic public health and medical enterprises. While that far-flung group offers opportunities for using local data in policy and practice, it also can result in an uneven allocation of resources and decision-making.
Public-health experts had been calling for a revamping of the American system even before COVID, but the pandemic “laid bare the deficiencies of the existing public health system and heightened the politicization of public health along partisan lines to an unworkable level in some jurisdictions,” the authors wrote, and highlighted the need for global collaboration.
The essay makes recommendations in seven areas of focus to guide public health transformation:
- Accountability: Provide as much transparency as possible in government actions, and share decisionmaking, budgeting and communication with community members.
- Politicization and polarization: Identify areas where there is consensus/common ground, make better use of local data and messengers, and establish legal protections from violence against public health workers.
- Climate change: Make climate change a core priority, develop ways to track its effects, and advocate for policies to address the root causes.
- Equity: Make health equity a core value of public health agencies, build skills among staff, fully engage the public and policymakers and address health and social needs in marginalized populations.
- Data sciences: Support the harmonization of data sets and repositories, enhance capacity, engage communities and develop real-time surveillance system to detect and monitor threats to public health.
- Workforce: Develop training in new areas, including resilience, communication, systems thinking and entrepreneurship.
- Communication: Identify distinct audiences, create messages that are positive and show benefits, translate evidence into easily understood stories, and identify “superspreaders” of misinformation.
- Follow us on Facebook
- Follow us on Twitter
- Criminal Justice
- Environment
- Politics & Government
- Race & Gender
Expert Commentary
Research highlights need for public health approach in news reporting of gun violence
The study, published in BMC Public Health, reveals an overwhelming reliance on law enforcement narratives, missing deeper insights into the root causes and potential solutions to gun violence.

Republish this article

This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License .
by Naseem S. Miller, The Journalist's Resource June 25, 2024
This <a target="_blank" href="https://journalistsresource.org/home/study-highlights-need-for-public-health-approach-in-news-reporting-of-gun-violence/">article</a> first appeared on <a target="_blank" href="https://journalistsresource.org">The Journalist's Resource</a> and is republished here under a Creative Commons license.<img src="https://journalistsresource.org/wp-content/uploads/2020/11/cropped-jr-favicon-150x150.png" style="width:1em;height:1em;margin-left:10px;">
For decades, researchers have urged journalists to avoid framing gun violence solely as a crime issue and provide a broader public health context. Yet, as evidenced by the findings of a recent study of local TV news in Philadelphia, the focus on the crime angle remains very much at the forefront of gun violence coverage.
The researchers’ call for change was further underscored on June 25, when the U.S. surgeon general declared firearm violence a public health crisis for the first time in a 40-page advisory , calling on the nation to take a public health approach to address gun violence, much like it has done before to address tobacco and car crashes.
In “ Public health framing of firearm violence on local television news in Philadelphia, PA, USA: a quantitative content analysis ,” published in BMC Public Health in May 2024, researchers analyzed 192 TV news clips aired on four local news stations between January and June 2021 and found that 84% contained at least one element that could be harmful to communities, audiences and gun violence survivors. Some of those elements are visuals of the crime scene, not following up on the story, naming the treating hospital and the relationship between the injured person and the shooter.
Meanwhile, public health elements such as root causes of gun violence, solutions and sources other than law enforcement officials were missing from most news clips.
“The main message is that the majority of reporting on firearm violence, at least in TV news, has many harmful content elements and we have to do better,” says the study’s lead author, Dr. Jessica Beard , director of research at The Philadelphia Center for Gun Violence Reporting, a trauma surgeon at Temple University Hospital and an associate professor at the Lewis Katz School of Medicine at Temple University. “The public does not have an accurate understanding of what gun violence is and the policy implications are huge.”
Beard was part of a panel on covering gun violence as a public health emergency at the Association of Health Care Journalists’ annual conference in New York City earlier this month. She also spoke with The Journalist’s Resource after the panel.
Previous studies have shown that when the news media covers community gun violence as a single incident in isolation, audiences are more likely to blame victims. This approach also reinforces racist stereotypes and suggests that policing is the most effective way to prevent violence, undermining public health measures that could curb gun violence, Beard and her co-authors of the BMC Public Health study write.
This type of coverage also has a negative effect on people who are injured in shootings , they point out.
Injured people say that graphic content, inaccuracies and mention of treating hospitals resulted in distress, harm to their reputation and threats to their personal safety, according to a 2023 study by the same research team, which included interviews with 26 adults who had recently sustained a gunshot wound. They said that news reports that neglected their personal perspectives left them feeling dehumanized and compounded their trauma.
“Some people were afraid to get discharged from the hospital,” Beard says.
More about the study and its findings
The researchers chose to study TV news because more people in the U.S. get their news from TV than other legacy sources such as radio and print, according to a 2023 survey by Pew Research Center. (That same survey found that more Americans get their news from digital devices than from TV, and there’s a need for research on firearm violence content in digital news, the authors note.)
They focus on Philadelphia for several reasons. The city is the birthplace of Eyewitness News, which launched in 1965, and Action News, which launched in 1970. The two newscasts pioneered reporting approaches that have been criticized for the way they are produced and for casting a negative light on Black communities, the authors write. A 2022 story by The Philadelphia Inquirer delves deep into this history.
Moreover, the epidemic of gun violence in Philadelphia reflects a trend across the country where shooting rates have increased since the onset of the COVID-19 pandemic, disproportionately affecting young people and Black people. A June report from the CDC’s Morbidity and Mortality Weekly Report finds that between January 2019 and September 2023, rates of emergency medical services encounters for gun-related injuries were highest among males, non-Hispanic Black people and people between 15 and 24 years old.
The study compares Philadelphia news clips based on two main characteristics: news clips that focused on a single incident in isolation, called episodic framing, and those with more of a public-health approach, exploring the broader social and structural context in which the violence occurs, called thematic framing.
Among the findings:
- Nearly 80% of the stories used episodic framing.
- In 21% of the clips, a law enforcement official was the main interview source.
- In 50.5% of the clips where the journalists were the only news narrators, police were the predominant source of information on firearm violence.
- More than 84% of the stories contained at least one harmful element, such as a visual of the crime scene, not following up on the story, the number of gunshot wounds, the name of the treating hospital and the relationship between the injured person and the shooter. About 7% of the clips included video or audio of the shooting.
- The 192 news clips mentioned a total of 433 injured people.
- More than 80% of the clips mentioned an injured person, although in 67%, the only information about injured people was age or gender.
- None of the 192 news segments included a health or public health professional or an injured person as the main interview source.
- Only 10% of the clips included discussions about public health solutions.
- And only five stories (2.6%) used the word “prevent.” Another four stories (2.1%) offered resources related to firearm prevention.
The authors point out that the study findings may not be generalizable to all U.S. cities, to national TV news, or to print, radio, or social media content.
Also, it’s still not clear whether harmful reporting on community firearm violence increases rates of gun violence. The connection between the two is complex, Beard says, adding that she’s hoping to explore and study the topic in the future.
In their 2023 study , Beard and colleagues asked injured participants if they would be willing to speak with a journalist about their shooting incident and what would they tell the journalist.
One participant said, “You report the gun violence, but why not do a follow-up report […] for the victims, the survivors, the families that had to bury these people, the whole process? Just don’t do a guy got shot over there, a guy got shot over here. You’re making people more fearful. You’re more fearful, you’re going to arm yourself more.”
The authors underscore the study participant’s point: Reporting on firearm violence with limited information and no follow-up stories may perpetuate fear, which may contribute to increasing firearm use and, in turn, the increasing incidence of firearm violence.
The BMC Public Health study was funded by the Stoneleigh Foundation, Lehigh University Research Investment Programs, the National Institute on Minority Health and Health Disparities of the National Institutes of Health, and the National Center for Injury Prevention and Control of the Centers for Disease Control and Prevention.
Gun violence as a public health issue
Two days after the Pulse nightclub mass shooting , where 49 people were killed by a lone gunman in Orlando, The American Medical Association adopted a policy calling gun violence “a public health crisis,” which requires a comprehensive public health response.
In addition to death, gun violence can result in long-term physical, mental and financial burdens among injured individuals, studies show, including a 2023 study published in JAMA Network Open. It impacts communities, causing fear and economic decline. And compared with infectious diseases, it poses a larger burden on society in terms of potential years of life lost, according to a 2020 report by the Educational Fund to Stop Gun Violence (now the Johns Hopkins Center for Gun Violence Solutions ).
Gun violence affects the health of entire communities, said Dr. Ruth Abaya , an attending physician in the Children’s Hospital of Philadelphia emergency department, during the panel on covering gun violence as a public health emergency at the Association of Health Care Journalists.
“We’re seeing young people who have crippling anxiety that is limiting their abilities to participate in daily life, they’re being medicated and even being hospitalized, and that’s directly related to this other public health crisis of gun violence,” said Abaya, who’s also the senior director of health systems and CVI — community violence intervention — integration at The Health Alliance for Violence Intervention. “And I’m also seeing young people with other unrelated chronic diseases like asthma that’s out of control because their caregiver was killed in a violent incident.”
Recommendations for journalists
The study’s findings are not surprising to Rick Brunson , a senior instructor of journalism at the University of Central Florida’s Nicholson School of Communication and Media.
Brunson, who worked as a reporter and editor in Central Florida for 20 years, including at a local TV station, mentions several reasons why many TV stations’ coverage of gun violence lacks a broader public health context.
Commercial news stations’ economic lifeblood depends on ratings, and as much as audiences may say they are put off by coverage of crime and violence, stations’ internal research shows that people watch crime news, he says.
Also, with the plethora of streaming options and multiple screens, viewers are distracted and TV stations are often vying for their attention, which results in newscasts packed with videos and short stories without space for context and explanation.
And there’s the broader, growing trend of news avoidance among audiences.
“When they watch the news, it just makes them feel despair and exhaustion, especially the focus on crime coverage and because there’s no context,” Brunson says. “They’re just presented with problem after problem after problem. Violence after violence.”
“The question for news directors to ask in the face of this where people are just avoiding the news and you’re seeing your audience erode more and more, year after year, is can the news business also be in the hope business?” Brunson says. “It’s going to take some serious consideration and the reversal of the kind of coverage that you put on your air.”
Even though there are widely accepted journalistic guidelines to protect victims and audiences in cases of suicide , mass shootings , sexual assault, abuse, and crime involving minors, no such guidelines crafted by journalists and public health practitioners exist for reporting on community firearm violence, Beard and her colleagues note in their study.
They say their research aims to lay the foundation for understanding harmful content in TV news clips and share several recommendations, including the practice of trauma-informed reporting.
Trauma-informed journalism recognizes the need for journalists to better understand how trauma can affect survivors and how to avoid reporting that could cause additional harm to vulnerable people and those who have experienced trauma. The practice also helps journalists to protect their own mental health.
When covering firearm violence, trauma-informed reporting would involve engaging with survivors using trauma-informed principles, including giving them control over the narrative of their injuries. It also minimizes harmful elements such as graphic visuals.
“This type of reporting could humanize firearm-injured people and build empathy in audiences, deconstructing the existing racialized news narratives around firearm violence in cities,” the authors write.
They also recommend:
- Public health practitioners partner with firearm violence survivors to offer alternative perspectives to journalists reporting on firearm violence.
- Journalists seek training in trauma-informed practices and solutions journalism .
- Newsrooms adopt a public health approach to reporting on firearm violence, provide resources to audiences and use the public health framing.
To help journalists and newsrooms meet these recommendations, the Philadelphia Center for Gun Violence Reporting and Frameworks Institute created a free gun violence reporting toolkit , which provides more information on trauma-informed reporting, the drivers of gun violence, and tips for more complete news coverage of gun violence.
Brunson advises reporters to seek out public health professionals as a source to help add context to their reporting and to read BMC Public Health study .
“People are always trying to tell us what to do,” Brunson says. “But we should take that as a compliment because the folks like the people who did this study acknowledge that they’re doing it because the media has influence, and journalists help shape and frame public debate and discussions and the problems that get looked at. Policymakers look at what journalists are doing.”
Additional research
Systematic disparities in reporting on community firearm violence on local television news in Philadelphia, PA, USA Jessica H. Beard, et al. Preventive Medicine Reports, April 2024.
“Like I’m a nobody:” firearm-injured peoples’ perspectives on news media reporting about firearm violence Jessica H. Beard, et al. Qualitative Research in Health, June 2023.
Firearm Injury — A Preventable Public Health Issue Jay Patel, et al. Lancet Public Health, November 2022.
Making the News: Victim Characteristics Associated with Media Reporting on Firearm Injury Elinore J Kaufman, et al. Preventive Medicine Reports, December 2020.
- To help journalists with better reporting of gun violence, PCGVR has created a free gun violence reporting toolkit .
- “ Firearm Violence: A Public Health Crisis in America ” is the U.S. Surgeon General’s 2024 advisory, a first of its kind for gun violence.
- The American Public Health Association’s Gun Violence page links to several useful resources.
- The Dart Center for Journalism & Trauma, the Canadian Broadcasting Corporation (CBC/Radio-Canada), and the Canadian Journalism Forum on Violence and Trauma recently launched a news industry toolkit on trauma-aware journalism.
- This fact sheet by the American Public Health Association lists some of the recommended public health responses to gun violence.
About The Author
Naseem S. Miller
A .gov website belongs to an official government organization in the United States.
A lock ( ) or https:// means you've safely connected to the .gov website. Share sensitive information only on official, secure websites.
- Current Situation
- Monitoring Current Situation
- Bird Flu in Animals and People
- Caring for Yourself and Others
- Avian Influenza Communication Resources
- Information for Specific Groups
- Case Definitions for Investigations of Human Infection with Avian Influenza A Viruses in the United States
- Clinical Overview
- Interim Guidance on the Use of Antiviral Medications for Treatment of Human Infections with Novel Influenza A Viruses Associated with Severe Human Disease
- Clinical Testing and Diagnosis
- Interim Guidance on Influenza Antiviral Chemoprophylaxis of Persons Exposed to Birds with Avian Influenza A Viruses Associated with Severe Human Disease or with the Potential to Cause Severe Human Disease
- Infection Control Guidance
- Considerations for Veterinarians: Evaluating and Handling of Cats Potentially Exposed to Highly Pathogenic Avian Influenza A(H5N1) Virus in Cats
- Conversation Tips: Unpasteurized (Raw Milk)
- H5N1 Bird Flu: Current Situation Summary
- Public Health Strategies for Bird Flu
- Novel Influenza A Guidance on Testing and Specimen Collection
- Interim Guidance for Follow-up of Close Contacts of Persons Infected with Novel Influenza A Viruses and Use of Antiviral Medications for Chemoprophylaxis
- H5N1 Technical Report
- Show All Home
CDC Public Health Science Agenda for Highly Pathogenic Avian Influenza A(H5N1) – June 2024
What to know.
- CDC has developed strategic priorities for improving global influenza control, prevention, preparedness, and response. These priorities guide research and surveillance activities around seasonal and pandemic influenza preparedness and response.
- CDC works to address these strategic priorities through ongoing collaboration with public and animal health partners at the local, state, and national level.
- CDC has identified the following primary HPAI A(H5N1) scientific response objectives for the current outbreak of HPAI A(H5N1) in dairy cattle, other animals, and people.
Beginning the week of March 25, 2024, the U.S. Department of Agriculture confirmed detections of highly pathogenic avian influenza HPAI A(H5N1) virus infection in dairy cows in the United States. On April 4, 2024, CDC initiated a center (National Center for Immunization and Respiratory Diseases)-led emergency response for the HPAI A(H5N1) outbreak in dairy cows with a One Health approach. Since April 2024, several human cases of H5N1 have been detected in association with the ongoing outbreak of HPAI A(H5N1) in dairy cows and other animals. Human infections have occurred in dairy workers who had direct exposure to cattle presumed to be infected with HPAI A(H5N1) virus ( H5N1 Bird Flu: Current Situation ).
The HPAI A(H5N1) viruses currently circulating in the United States have thus far not demonstrated the ability to efficiently bind to receptors that predominate in the human upper respiratory tract. This is a major reason why CDC assesses the current risk to the public from HPAI A(H5N1) viruses to be low. However, influenza viruses have potential to rapidly evolve and HPAI A(H5N1) viruses are widely prevalent globally in wild birds. Therefore, continued comprehensive and coordinated, multisectoral surveillance across public health and animal health for these viruses in wild birds, poultry, mammals, and people worldwide, are critical to determine the public health risk.
CDC has developed strategic priorities for improving global influenza control, prevention, preparedness, and response. These priorities guide research and surveillance activities around seasonal and pandemic influenza preparedness and response. CDC works to address these strategic priorities through ongoing collaboration with public and animal health partners at the local, state, and national level. Additionally, CDC has identified the following primary HPAI A(H5N1) scientific response objectives for the current outbreak of HPAI A(H5N1) in dairy cattle, other animals, and people.
Objective 1
Prevent infection and illness in people exposed to hpai a(h5n1) viruses..
Focus Area: Understanding the risk of infection among people exposed to infected dairy cattle, other animals, and their environment or contaminated animal products (e.g., raw milk).
Focus Area: Determining what measures most minimize the risk of infection among exposed persons. This includes personal protective equipment (PPE), and administrative and engineering controls.
Focus Area: Identifying host, pathogen, and exposure risk indicators for severe illness.
Focus Area: Monitoring and evaluating the effectiveness of influenza antiviral medications in preventing and attenuating illness, and public health interventions, including A(H5N1) vaccine (should it be employed).
Objective 2
Understand human infection and illness with hpai a(h5n1) virus (clinical, virologic, and epidemiologic characteristics)..
Focus Area: Monitoring for human infections using existing influenza surveillance platforms and developing strategies for enhanced surveillance and laboratory testing.
Focus Area: Determining how widespread human exposure and infection are. This includes estimating the prevalence and incidence of human infections.
Focus Area: Identifying the primary means of transmission for HPAI A(H5N1) human infections. This includes animal-to-human zoonotic transmission and transmission via fomites. It also includes assessment of how the virus gains entry and replicates in humans.
Focus Area: Describing the spectrum of human clinical illness, including prevalence of severe illness, illness resulting in hospitalization or death, and asymptomatic and pauci-symptomatic cases.
Focus Area: Describing parameters important to human infection and resolution of illness, including estimated incubation period and duration of infectiousness.
Focus Area: Employing animal models to help describe clinical presentation, virulence, and transmissibility of these HPAI A(H5N1) viruses compared to seasonal and other zoonotic influenza viruses.
Focus Area: Identifying virologic characteristics of HPAI A(H5N1) viruses. Identifying genetic markers associated with increased infectivity, transmissibility or reduced antiviral susceptibility. Tracking genetic changes that occur in the virus during animal and human infections.
Objective 3
Prepare for and mitigate the possibility of an hpai a(h5n1) virus pandemic..
Focus Area: Estimating the pandemic potential of this HPAI A(H5N1) virus with the Influenza Risk Assessment Tool (IRAT) .
Focus Area: Conducting comprehensive antigenic, phenotypic, genotypic, and evolutionary characterization of HPAI A(H5N1) viruses detected in humans and animals.
Focus Area: Identifying candidate vaccine viruses (CVVs) expected to provide protection against currently circulating HPAI A(H5N1) viruses in animals; evaluating antiviral drugs to assess emergence of drug resistant viruses; and developing diagnostic test methods and additional assays to rapidly and accurately identify HPAI A(H5N1) virus infections.
Focus Area: Estimating the impact of nonpharmaceutical interventions and medical counter measures, including pre-pandemic H5 vaccines and potential H5 vaccines made using existing candidate vaccine viruses in preventing infection and/or severe illness, should widespread person-to-person transmission occur.
Focus Area: Coordinating with the WHO's Global Influenza Programme and the Global Influenza Surveillance and Response System (GISRS) and the OFFLU animal health network (World Organisation for Animal Health, Food and Agriculture Organization, and reference laboratories) to support rapid information and resource sharing. As a WHO Influenza Collaborating Centre, the CDC Influenza Division actively supports global surveillance efforts and contributes materials, technical assistance, and data to global veterinary and public health partners to guide pandemic preparedness planning, including development/deployment of H5 diagnostic tests, monitoring for antiviral resistance, recommendations/development of vaccine candidates, and virus risk assessment.
Focus Area: Conducting immunologic and virologic pandemic risk assessment of novel influenza viruses in animal models and other model system.
Focus Area: Determining virus and host factors that impact virulence and transmission of novel influenza viruses, including conducting serology studies to determine the population immunity among the general population to HPAI A(H5N1) viruses.
Focus Area: Evaluating strategies to increase uptake of public health interventions such as vaccines.
Avian influenza or bird flu refers to the disease caused by infection with avian (bird) influenza (flu) Type A viruses.
For Everyone
Health care providers, public health.
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
- My Bibliography
- Collections
- Citation manager
Save citation to file
Email citation, add to collections.
- Create a new collection
- Add to an existing collection
Add to My Bibliography
Your saved search, create a file for external citation management software, your rss feed.
- Search in PubMed
- Search in NLM Catalog
- Add to Search
The values and risks of an Intergovernmental Panel for One Health to strengthen pandemic prevention, preparedness, and response
Affiliations.
- 1 UMR MoISA, CIRAD, Montpellier, France; MoISA, University of Montpellier, Montpellier, France; CIHEAM-IAMM, INRAE, Institut Agro, Montpellier, France.
- 2 Geneva Science-Policy Interface, University of Geneva, Geneva, Switzerland; Simon Institute for Longterm Governance, Geneva, Switzerland.
- 3 Department of Health Security, Finnish Institute for Health and Welfare, Helsinki, Finland.
- 4 Department of Biomedical Sciences, Institute of Tropical Medicine, Antwerp, Belgium.
- 5 Institute for Environmental Sciences, University of Geneva, Geneva, Switzerland.
- 6 Institute of Anthropology, Gender and African Studies, University of Nairobi, Nairobi, Kenya.
- 7 Graduate Institute of International and Development Studies, Geneva, Switzerland.
- 8 Swiss Tropical and Public Health Institute, Allschwil, Switzerland; Human and Animal Health Unit, University of Basel, Basel, Switzerland.
- 9 Centre for Viral Zoonoses, Department of Medical Virology, Faculty of Health Sciences, University of Pretoria, Pretoria, South Africa.
- 10 Department of Biological Safety, German Federal Institute for Risk Assessment (BfR), Berlin, Germany.
- 11 Swiss Agency for Development and Cooperation, Bern, Switzerland.
- 12 Research Institute for Development, PREZODE Initiative, Montpellier, France.
- 13 BIOS/UMR ASTRE, CIRAD, Montpellier, France.
- 14 Empa-Swiss Federal Laboratories for Materials Science and Technology, Technology and Society Laboratory, St Gallen, Switzerland.
- 15 Geneva Science-Policy Interface, University of Geneva, Geneva, Switzerland.
- 16 Department of Public Health, Institute of Tropical Medicine, Antwerp, Belgium; Julius Center for Health Sciences and Primary Care, Utrecht University, Utrecht, Netherlands. Electronic address: [email protected].
- PMID: 37474236
- DOI: 10.1016/S2214-109X(23)00246-2
The COVID-19 pandemic has shown the need for better global governance of pandemic prevention, preparedness, and response (PPR) and has emphasised the importance of organised knowledge production and uptake. In this Health Policy, we assess the potential values and risks of establishing an Intergovernmental Panel for One Health (IPOH). Similar to the Intergovernmental Panel on Climate Change, an IPOH would facilitate knowledge uptake in policy making via a multisectoral approach, and hence support the addressing of infectious disease emergence and re-emergence at the human-animal-environment interface. The potential benefits to pandemic PPR include a clear, unified, and authoritative voice from the scientific community, support to help donors and institutions to prioritise their investments, evidence-based policies for implementation, and guidance on defragmenting the global health system. Potential risks include a scope not encompassing all pandemic origins, unclear efficacy in fostering knowledge uptake by policy makers, potentially inadequate speed in facilitating response efforts, and coordination challenges among an already dense set of stakeholders. We recommend weighing these factors when designing institutional reforms for a more effective global health system.
Copyright © 2023 The Author(s). Published by Elsevier Ltd. This is an Open Access article under the CC BY-NC-ND 4.0 license. Published by Elsevier Ltd.. All rights reserved.
PubMed Disclaimer
Conflict of interest statement
Declaration of interests We declare no competing interests.
Similar articles
- National and subnational governance and decision-making processes during the COVID-19 pandemic in Nigeria: an empirical analysis. Mukherjee S, Asthana S, Ukponu W, Ihueze AC, Gobir IB, Phelan AL, Standley CJ. Mukherjee S, et al. BMJ Glob Health. 2023 Sep;8(9):e012965. doi: 10.1136/bmjgh-2023-012965. BMJ Glob Health. 2023. PMID: 37696545 Free PMC article.
- Embed Multisectoral Governance Mechanisms in the Pandemic Instrument for One Health Action. Palkovits M, Van Katwyk SR, Hoffman SJ. Palkovits M, et al. J Law Med Ethics. 2022;50(S2):71-81. doi: 10.1017/jme.2023.30. J Law Med Ethics. 2022. PMID: 36889347 Free PMC article.
- Pandemic origins and a One Health approach to preparedness and prevention: Solutions based on SARS-CoV-2 and other RNA viruses. Keusch GT, Amuasi JH, Anderson DE, Daszak P, Eckerle I, Field H, Koopmans M, Lam SK, Das Neves CG, Peiris M, Perlman S, Wacharapluesadee S, Yadana S, Saif L. Keusch GT, et al. Proc Natl Acad Sci U S A. 2022 Oct 18;119(42):e2202871119. doi: 10.1073/pnas.2202871119. Epub 2022 Oct 10. Proc Natl Acad Sci U S A. 2022. PMID: 36215506 Free PMC article. Review.
- Analyzing the Characteristics of Policies and Political Institutions for the Prevention and Control Governance of the COVID-19 Pandemic: Evidence from China. Dong M, Zhou C, Zhang Z. Dong M, et al. Int J Environ Res Public Health. 2022 Sep 2;19(17):10980. doi: 10.3390/ijerph191710980. Int J Environ Res Public Health. 2022. PMID: 36078703 Free PMC article.
- Pharmacy Emergency Preparedness and Response (PEPR): a proposed framework for expanding pharmacy professionals' roles and contributions to emergency preparedness and response during the COVID-19 pandemic and beyond. Aruru M, Truong HA, Clark S. Aruru M, et al. Res Social Adm Pharm. 2021 Jan;17(1):1967-1977. doi: 10.1016/j.sapharm.2020.04.002. Epub 2020 Apr 10. Res Social Adm Pharm. 2021. PMID: 32389631 Free PMC article. Review.
- Multi-country case study on school health policy and its implementation in relation to COVID-19 control in Micronesia Small Islands Developing States. Shibuya F, Hattori-Uchima M, Dacanay P, Peter F, Ngirmang TT, Dacanay R, Takeuchi R, de Los Reyes C, Kobayashi J. Shibuya F, et al. Trop Med Health. 2024 Mar 29;52(1):27. doi: 10.1186/s41182-024-00590-8. Trop Med Health. 2024. PMID: 38553741 Free PMC article.
Publication types
- Search in MeSH
Related information
Linkout - more resources, full text sources.
- Elsevier Science
- MedlinePlus Health Information

- Citation Manager
NCBI Literature Resources
MeSH PMC Bookshelf Disclaimer
The PubMed wordmark and PubMed logo are registered trademarks of the U.S. Department of Health and Human Services (HHS). Unauthorized use of these marks is strictly prohibited.
Information
- Author Services
Initiatives
You are accessing a machine-readable page. In order to be human-readable, please install an RSS reader.
All articles published by MDPI are made immediately available worldwide under an open access license. No special permission is required to reuse all or part of the article published by MDPI, including figures and tables. For articles published under an open access Creative Common CC BY license, any part of the article may be reused without permission provided that the original article is clearly cited. For more information, please refer to https://www.mdpi.com/openaccess .
Feature papers represent the most advanced research with significant potential for high impact in the field. A Feature Paper should be a substantial original Article that involves several techniques or approaches, provides an outlook for future research directions and describes possible research applications.
Feature papers are submitted upon individual invitation or recommendation by the scientific editors and must receive positive feedback from the reviewers.
Editor’s Choice articles are based on recommendations by the scientific editors of MDPI journals from around the world. Editors select a small number of articles recently published in the journal that they believe will be particularly interesting to readers, or important in the respective research area. The aim is to provide a snapshot of some of the most exciting work published in the various research areas of the journal.
Original Submission Date Received: .
- Active Journals
- Find a Journal
- Proceedings Series
- For Authors
- For Reviewers
- For Editors
- For Librarians
- For Publishers
- For Societies
- For Conference Organizers
- Open Access Policy
- Institutional Open Access Program
- Special Issues Guidelines
- Editorial Process
- Research and Publication Ethics
- Article Processing Charges
- Testimonials
- Preprints.org
- SciProfiles
- Encyclopedia

Article Menu

- Subscribe SciFeed
- Google Scholar
- on Google Scholar
- Table of Contents
Find support for a specific problem in the support section of our website.
Please let us know what you think of our products and services.
Visit our dedicated information section to learn more about MDPI.
JSmol Viewer
Exploring the nature of diversity dishonesty within predominantly white schools of medicine, pharmacy, and public health at the most highly selective and highly ranked u.s. universities.

Share and Cite
Burrell, D.N. Exploring the Nature of Diversity Dishonesty within Predominantly White Schools of Medicine, Pharmacy, and Public Health at the Most Highly Selective and Highly Ranked U.S. Universities. Soc. Sci. 2024 , 13 , 332. https://doi.org/10.3390/socsci13070332
Burrell DN. Exploring the Nature of Diversity Dishonesty within Predominantly White Schools of Medicine, Pharmacy, and Public Health at the Most Highly Selective and Highly Ranked U.S. Universities. Social Sciences . 2024; 13(7):332. https://doi.org/10.3390/socsci13070332
Burrell, Darrell Norman. 2024. "Exploring the Nature of Diversity Dishonesty within Predominantly White Schools of Medicine, Pharmacy, and Public Health at the Most Highly Selective and Highly Ranked U.S. Universities" Social Sciences 13, no. 7: 332. https://doi.org/10.3390/socsci13070332
Article Metrics
Article access statistics, further information, mdpi initiatives, follow mdpi.

Subscribe to receive issue release notifications and newsletters from MDPI journals
Public ranks long-term challenges and health determinants as top priorities for new EU
To enhance public health, the post-election European Union (EU) should prioritise long-term challenges such as climate change and the ageing population, as well as factors that influence our health, according to a new report . The findings, derived from a seven-month public debate led by the European Observatory on Health Systems and Policies, highlight a collective call for the EU to play a more significant role in health.
The report, which is based on the public debate commissioned by the European Commission’s Directorate General for Health and Food Safety ( DG SANTE ), outlines the key priorities and actions desired by citizens and stakeholders from a wide range of sectors and mostly from Europe. The analysis included more than 800 responses in conference polls and a survey, plus comprehensive inputs across three webinars .
The large and participatory initiative allowed to collect public opinion on nine critical health topics: health security; determinants of health; health system transformation; the health workforce; universal health coverage; digital solutions and AI; performance and resilience; long-term challenges like climate change and ageing; and the EU’s global role in health.
The public’s calls for action – including across sectors
Participants called for the European Commission to coordinate across its different policy branches. Collaborating across sectors is considered key to deliver health priorities, making the concepts of ‘ Health in All Policies’ and ‘Health for All Policies ’ important tools for addressing the determinants of health. Interestingly, the topics which garnered the highest consensus in the discussion framework were those least controlled by the health sector alone.
Significant measures should be taken to mitigate the health impacts of environmental risks, including promoting environmental health and supporting health equity through integrated policies. Participants also considered addressing the needs of an ageing population essential, by improving health services and ensuring that health systems are prepared to meet the demands of older adults.
The public opinion suggested several actions to achieve universal health coverage (UHC) across the EU, such as ensuring equal access to comprehensive health care services for all EU citizens and financial protection for all. Other recommendations ranged from establishing a common minimum coverage package and a European health insurance scheme to focusing on underserved groups, improving health literacy, and including mental health in UHC policies.
What role for the EU?
Participants highlighted the importance of EU legal frameworks and instruments in promoting and safeguarding health, such as funding and technical support. They advocated both for new tools and for better implementation and coordination of existing mechanisms.
Aligning educational standards was raised as a key topic in the context of addressing shortages of health workers , regional disparities and managing the demands for new skills. Better addressing health workforce needs and improving their working conditions to mitigate existing gaps was also discussed. There was consensus on the need for EU approaches to health workforce issues, including better coordination of initiatives and pursuit of EU wide policies.
Digital solutions , health security and strengthening the EU’s global voice and leadership were widely discussed but ranked slightly lower. Possible explanations outlined in the report include the “transversal nature of digital solutions, which voters may have perceived as a means to achieving other priorities”. The COVID-19 pandemic and sustained EU action on health security may have elicited some voters to opt for other topics that have received less policy attention in recent years.
Survey, webinars, and conference polls
Media Contacts
Débora Miranda
Communications and Dissemination Officer
Subscribe to our newsletter

COMMENTS
151+ Public Health Research Topics [Updated 2024] The important area of public health research is essential to forming laws, influencing medical procedures, and eventually enhancing community well-being. As we delve into the vast landscape of public health research topics, it's essential to understand the profound impact they have on society.
Discover the articles that are trending right now, and catch up on current topics in Public Health and related disciplines. We will update our collection every few weeks; come back to this page to be on top of the latest conversations in Public Health and Medicine. Previously featured articles are listed here.
If you're still unsure about how to find a quality research topic, check out our Research Topic Kickstarter service, which is the perfect starting point for developing a unique, well-justified research topic. A comprehensive list of public health-related research topics. Includes free access to a webinar and research topic evaluator.
New Environmental Pollutants, Aging, and Age-Related Diseases. Lai Xuefeng. Ling Zhang. Wending Li. Yi Wang. 417 views. The most cited cited journal in its field, which promotes discussion around inter-sectoral public health challenges spanning health promotion to climate change, transportation, environmental change...
Public Health Challenges is a multidisciplinary journal addressing all areas of public health research, policy, and practice, and supporting the One Health agenda. Abstract We identify ten public health challenges that need to be closely tracked in 2022. These challenges are COVID-19, inadequate human resources for health, poor health systems ...
The Fogarty International Center and its NIH partners invest in research on a variety of topics vital to global health. For each of these global health research topics, find an in-depth collection of news, resources and funding from Fogarty, the NIH, other U.S. government agencies, nongovernmental organizations and others. Bioethics.
Public Health Challenges is a multidisciplinary journal addressing all areas of public health research, policy, and practice, and supporting the One Health agenda. Abstract The year 2022 saw COVID-19 as the primary public health concern, with vaccine rollout and mandates at the forefront.
Public health is the medical discipline concerned with the prevention and control of disease through population surveillance and the promotion of healthy behaviours. ... A growing body of research ...
2021 has been an unprecedented year in public health. We entered the second calendar year of dealing with a pandemic that has devastated global health infrastructures, widened health inequalities, and exposed health system vulnerabilities. The ongoing COVID-19 pandemic has also significantly set back Sustainable Development Goal 3 (SDG 3 - Good Health and Well Being) progress, in particular ...
In this Research Topic we present a few examples of applications of the epidemiological and public health methods to address emerging societal issues, that require bright policy solutions. Needless to say, the relationship between science and policy is not straightforward. It would be naïve to think that scientists provide evidence and then ...
Here, we'll explore a variety of healthcare-related research ideas and topic thought-starters across a range of healthcare fields, including allopathic and alternative medicine, dentistry, physical therapy, optometry, pharmacology and public health. NB - This is just the start….
According to the World Health Organization (WHO), public health is "the art and science of preventing diseases, helping to prolong life and promote health using organized efforts. Good examples of public health efforts include preventing outbreaks, educating the public on health choices, promoting fitness, preparing for emergencies, and ...
Project Duration. 2022-07-18 — 2025-07-30. Methodology and Advanced Analytics Resource Center. Principal Investigator. Boodram, Basmattee. Funding Source. National Institute of Drug Abuse (National Institutes of Health) Reducing Opioid Mortality in Illinois. Principal Investigator.
Data science is a newly‐formed and, as yet, loosely‐defined discipline that has nonetheless emerged as a critical component of successful scientific research. We seek to provide an understanding of the term "data science," particularly as it relates to public health; to identify ways that data science methods can strengthen public ...
Research. Strategy and Development; Implementation and Impact; Integrity and Oversight; Practice. In the School; ... Topics. Our topic pages offer a one-stop-shop for insights, experts, and offerings by areas of interest. ... Johns Hopkins Bloomberg School of Public Health 615 N. Wolfe Street, Baltimore, MD 21205. Footer social. LinkedIn ...
Public health research topics are areas of study within the larger field of public health. They cover diverse issues like community health, disease prevention, and health policies. These research topic ideas help us understand and improve global healthcare. They can explore various factors like environmental impacts on public overall wellbeing ...
The politicization of public health and the impact on health officials and the workforce: charting a path forward. Am J Public Health. 2022;112 (5):734-5. Crossref, Medline , Google Scholar. 5 ...
Consider the following key public health topics for research in 2023 and beyond. Public Health Research Topics for 2023. Every researcher's goal is to uncover important information that can be used to determine potential solutions to help address specific health issues. Public health researchers consider the potential impact of their research ...
Public health is a broad field. We focus on the most important problems and solutions of our time. Check back often to see what topics and issues we're working on. Aging, Health and Equity. Chronic Disease. Climate, Health and Equity. Communicable Disease. Community Water Fluoridation. COVID-19.
Artificial intelligence (AI) has the potential to revolutionize research by automating data analysis, generating new insights, and supporting the discovery of new knowledge. The top 10 contribution areas of AI towards public health were gathered in this exploratory study. We utilized the "text-davinci-003" model of GPT-3, using OpenAI ...
In the funding of health research and public health research, it is essential that the research questions addressed are important to patients and the health of the public, and that funded research meets a research need or a gap in evidence [1, 2].It is also vital that there is a connection between policy, practice and research [3, 4].The identification of research needs is a complex task, with ...
The following Research Topics are led by experts in their field and contribute to the scientific understanding of public-health. These Research topics are published in the peer-reviewed journal Frontiers in Public Health, as open access articles.
The public health system in the United States needs an immediate "transformation," two of the nation's leading health experts write in a new appeal for change driven by the COVID-19 pandemic, climate change, and the politicization of public health. The essay is the lead article in "Reimagining Public Health," a new special issue of Health Affairs, one of
Vitamin D receptors are expressed in many organs and tissues, which suggests that vitamin D (VD) affects physiological functions beyond its role in maintaining bone health. Deficiency or inadequacy of 25(OH)VD is widespread globally. Population studies demonstrate that a positive association exists between a high incidence of VD deficiency and a high incidence of chronic diseases, including ...
A Philadelphia Inquirer video explains how Eyewitness News and Action News brands of TV news, born in Philadelphia, harmed Black America.. Gun violence as a public health issue. Two days after the Pulse nightclub mass shooting, where 49 people were killed by a lone gunman in Orlando, The American Medical Association adopted a policy calling gun violence "a public health crisis," which ...
CDC works to address these strategic priorities through ongoing collaboration with public and animal health partners at the local, state, and national level. Additionally, CDC has identified the following primary HPAI A(H5N1) scientific response objectives for the current outbreak of HPAI A(H5N1) in dairy cattle, other animals, and people.
The potential benefits to pandemic PPR include a clear, unified, and authoritative voice from the scientific community, support to help donors and institutions to prioritise their investments, evidence-based policies for implementation, and guidance on defragmenting the global health system. Potential risks include a scope not encompassing all ...
The concept of "diversity dishonesty" has emerged as a pressing concern within highly selective and highly ranked schools of medicine, pharmacy, and public health at elite and highly ranked U.S. universities, particularly in the context of diversity, equity, and inclusion (DEI) efforts. This phenomenon, defined as a lack of sincerity and genuineness in an organization's commitment to ...
To enhance public health, the post-election European Union (EU) should prioritise long-term challenges such as climate change and the ageing population, as well as factors that influence our health, according to a new report. The findings, derived from a seven-month public debate led by the European Observatory on Health Systems and Policies, highlight a collective call for the EU to play a ...
As part of the study, the researchers used information held by ICES on health service use and other linked data to examine previous mental health use in Ontarians aged 15-29 years who were later ...